Committee on the Budget
House of Representatives
United States Government Accountability Office
A report to the Chairman, Committee on the Budget, House of Representatives
For more information, contact: Leslie V. Gordon at GordonLV@gao.gov
What GAO Found
The Center for Medicare and Medicaid Innovation (Innovation Center) was established within the Centers for Medicare & Medicaid Services (CMS) to test new approaches to health care delivery and payment—known as models—for use in Medicare or Medicaid. From 2011 through 2024, the Innovation Center obligated $11.4 billion for its activities. These included the testing of 70 models—24 of which were actively being tested as of January 2025. Total annual obligations peaked at $1.3 billion in fiscal year 2015 and have since decreased by nearly 40 percent to $789 million in fiscal year 2024. According to officials, these trends reflect the number of models the Innovation Center tests, among other factors.
Center for Medicare and Medicaid Innovation (Innovation Center) General Process for Model Development and Testing

Of 70 models tested, the Innovation Center has expanded four models to be implemented nationwide. These four models achieved net savings during the testing period. In addition to expanding certain models, the Innovation Center has also incorporated elements into Medicare and tested successor models that iterate upon previous concepts.
The Innovation Center uses selected performance management practices to regularly assess the performance of its efforts to test new health care delivery and payment approaches. For example, in May 2025, the Innovation Center established new long-term goals to outline the agency’s vision for its activities. It also developed corresponding near-term goals, including performance measures with targets and time frames. The Innovation Center uses this information to evaluate its progress toward its long-term goals, according to officials, and plans to regularly assess the outcomes of its activities against these near-term goals.
Why GAO Did This Study
In 2010, the Patient Protection and Affordable Care Act established the Innovation Center to test new health care delivery and payment approaches to reduce federal health spending. In 2012 and 2018, GAO reported on the Innovation Center’s progress in testing models, use of resources, and its assessment of its overall performance.
GAO was asked to update its earlier work. In this report, GAO (1) describes the Innovation Center’s obligations from 2011 through 2024 and how it obligated the funds to develop and test models; (2) describes the outcomes of model testing; and (3) examines the extent to which the Innovation Center follows selected practices of performance management to assess its performance.
GAO reviewed obligations data from fiscal years 2011 through 2024, reviewed model documentation and performance information, and compared efforts against selected performance management practices. GAO interviewed officials from the Innovation Center and CMS’s Office of the Actuary.
Abbreviations
|
ACO |
accountable care organization |
|
CBO |
Congressional Budget Office |
|
CHIP |
Children’s Health Insurance Program |
|
CMS |
Centers for Medicare & Medicaid Services |
|
HHS |
Department of Health and Human Services |
|
Innovation Center |
Center for Medicare and Medicaid Innovation |
|
PPACA |
Patient Protection and Affordable Care Act |
|
PTAC |
Physician-Focused Payment Model Technical Advisory Committee |
This is a work of the U.S. government and is not subject to copyright protection in the United States. The published product may be reproduced and distributed in its entirety without further permission from GAO. However, because this work may contain copyrighted images or other material, permission from the copyright holder may be necessary if you wish to reproduce this material separately.
March 27, 2026
The Honorable Jodey Arrington
Chairman
Committee on the Budget
House of Representatives
Dear Mr. Chairman:
Federal spending on Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP) is expected to reach $1.6 trillion in fiscal year 2025 and to continue increasing.[1] In 2010, the Patient Protection and Affordable Care Act (PPACA) established the Center for Medicare and Medicaid Innovation (Innovation Center), within the Centers for Medicare & Medicaid Services (CMS), to reduce federal health care spending as well as improve quality of care for beneficiaries.[2] To do so, the Innovation Center is tasked with testing new ways for delivering and paying for services. Specifically, the Innovation Center operates and evaluates pilot programs—known as models—to test the effects of new health care delivery and payment approaches in Medicare, Medicaid, and CHIP.[3]
The law provided a dedicated appropriation for testing models—$10 billion for the Innovation Center’s activities for fiscal years 2011 through 2019 and $10 billion per decade beginning in fiscal year 2020.[4] In addition, the law provided CMS, within the Department of Health and Human Services (HHS), with authority to expand the duration and scope of successful models through rulemaking.
Though initially projected to produce net savings, in September 2023, the Congressional Budget Office (CBO) determined that the Innovation Center had increased federal spending by $5.4 billion from fiscal years 2011 through 2020.[5] Specifically, CBO estimated that the Innovation Center spent $7.9 billion to operate models and those models reduced federal health care spending by $2.6 billion during this period. CBO noted its initial projection involved considerable uncertainty because of the lack of available data. After further reviewing the Innovation Center’s model activities, CBO subsequently projected that the Innovation Center would increase federal spending by $1.3 billion from fiscal years 2021 through 2030.
We previously reported on the Innovation Center. In November 2012, we reported on the Innovation Center’s early activities following its establishment.[6] In March 2018, we reported on the Innovation Center’s progress in testing models, its use of resources to operate the Innovation Center, and its assessment of its overall performance.[7] We found that the Innovation Center had tested 37 models as of March 2018 and used the evaluation results to make changes to models and to inform the development of new models. We also found that the Innovation Center had reported meeting targets for some of its performance goals as of 2015.
You asked us to update our previous work and to provide information on the activities of the Innovation Center. In this report we
1. describe the Innovation Center’s obligations from 2011 through 2024 and how it obligated the funds to develop and test models;
2. describe the outcomes of model testing undertaken by the Innovation Center as of January 2025; and
3. examine the extent to which the Innovation Center follows selected practices of performance management to assess its performance.
To describe the Innovation Center’s obligations from 2011 through 2024 and how it obligated the funds to develop and test models, we analyzed data provided by CMS on Innovation Center obligations under section 1115A of the Social Security Act by year and by category. Fiscal year 2024 was the most recent year of data available at the time of analysis. We also reviewed the Innovation Center’s model summary data and model documentation to identify the models operated from January 2011 through January 2025 and to compile information on the key characteristics of these models.[8] We included models tested under section 1115A and those that were statutorily required.[9] In addition, we reviewed CMS data on the model participants (such as health care provider organizations or states) for models operated as of January 2025. We also interviewed and obtained written responses from CMS officials about its obligations and model testing activities. We assessed the reliability of the obligation data by comparing it to outlays reported by CBO in September 2023, to obligations data reported in our previous work on the Innovation Center, and to obligations reported in the Innovation Center’s biennial reports to Congress.[10] We assessed the reliability of the model summary data and model participants data by comparing it to model documentation. We also obtained written responses regarding these data from CMS officials. We determined all these data were sufficiently reliable for the purposes of describing the Innovation Center’s obligations and how it obligated funds to develop and test models.
To describe the outcomes of model testing undertaken by the Innovation Center, we reviewed CMS Innovation Center and CMS Office of the Actuary documentation of model outcomes, including those related to model evaluations, model expansion, and how information on model performance was used. From model evaluations, we compiled information on health care participant attrition—including the change in participation during testing and reasons participants cited for dropping out. Specifically, we reviewed information on the attrition of participating health care provider organizations for models that have concluded testing and for which a final evaluation, with results for the entire test period, was available as of March 2025. We also reviewed model documentation and the Innovation Center’s biennial reports to Congress to identify successor models that were influenced by prior models among the models active as of January 2025. Additionally, we reviewed the Innovation Center’s biennial reports to Congress and publications synthesizing the results of model testing to obtain information about factors that affect the potential to achieve savings during model testing. We interviewed and obtained written responses from Innovation Center officials and Office of the Actuary officials regarding model outcomes and how information on model outcomes is used.
To evaluate the extent to which the Innovation Center follows selected practices of performance management, we reviewed Innovation Center documentation related to its goals and assessment of its performance for 2025 and its plans moving forward. We also interviewed and obtained written responses from CMS officials on the Innovation Center’s efforts for assessing program performance. We evaluated the Innovation Center’s efforts to assess its performance by comparing the agency’s activities to three selected practices for performance management.[11] We selected the most relevant practices among those identified in our prior work. These practices are (1) establishing long-term goals that communicate the results that an agency seeks to achieve, (2) establishing near-term goals that define expected results in the near-term and that include performance measures, and (3) using performance information to assess results.
We conducted this performance audit from November 2024 to March 2026 in accordance with generally accepted government auditing standards. Those standards require that we plan and perform the audit to obtain sufficient, appropriate evidence to provide a reasonable basis for our findings and conclusions based on our audit objectives. We believe that the evidence obtained provides a reasonable basis for our findings and conclusions based on our audit objectives.
Background
Requirements for Models
Section 1115A establishes certain requirements for the Innovation Center that relate to the selection of models, use of resources, and evaluation of models. These requirements include the following:
· Consulting with representatives of relevant federal agencies, as well as clinical and analytical experts in medicine or health care management, when carrying out its duties as described in the law.
· Ensuring models address deficits in care that have led to poor clinical outcomes or potentially avoidable spending.
· Making no less than $25 million of the Innovation Center’s dedicated funding available for model design, implementation, and evaluation each fiscal year starting in 2011.
· Evaluating each model to analyze its effects on spending and quality of care and making these evaluations public.
· Modifying or terminating a model unless it determines after testing has begun that the model either improves quality of care without increasing spending levels, reduces spending without reducing quality, or both.
In addition, certain requirements previously cited by the Medicare Payment Advisory Commission as administrative barriers to the timely completion of demonstrations are inapplicable.[12] Specifically, section 1115A provides the following:
· CMS cannot require that an Innovation Center model initially be budget neutral—that is, designed so that estimated federal expenditures under the model are expected to be no more than they would have been without the model—prior to approving a model for testing.
· Certain CMS actions in testing and expanding Innovation Center models such as the termination or modification of a model cannot be subject to administrative or judicial review.
· The Paperwork Reduction Act—which generally requires agencies to submit all proposed information collection efforts to the Office of Management and Budget for approval and provides a 60-day period for public comment when agencies want to collect data on 10 or more individuals—does not apply to Innovation Center models.[13]
Model Development and Testing Process
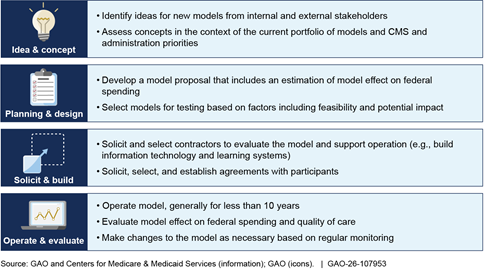
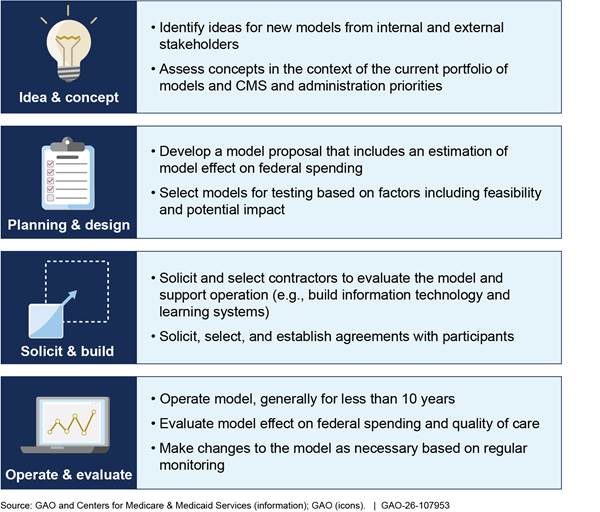
The Innovation Center generally follows four phases to develop and test a model.[14] (See fig. 1.)
Figure 1: Center for Medicare and Medicaid Innovation (Innovation Center) General Process for Model Development and Testing
|
Physician-Focused Payment Model Technical Advisory Committee (PTAC) PTAC reviewed and made recommendations to the Secretary of Health and Human Services on 28 stakeholder model proposals from 2017 through 2020. Of the 28 proposals, PTAC recommended 20 proposals for testing or other consideration. The Center for Medicare and Medicaid Innovation (Innovation Center) has cited nine of the proposals recommended by PTAC as influencing six models it has tested, though it has not tested any of the PTAC proposals in full. For example, one proposal influenced several elements of the Kidney Care Choices Model, including a provider bonus for successful kidney transplants and a focus on care coordination. Several proposals influenced three primary care models—Primary Care First, Making Care Primary, and Global Professional and Direct Contracting. For instance, based on one proposal, the Making Care Primary Model created payment codes to incentivize electronic consultations and care coordination, according to CMS officials. In addition, multiple oncology-related proposals influenced the Oncology Care and Enhancing Oncology models. While PTAC has not received new proposal submissions from stakeholders since 2020, it has continued to gather information from stakeholders—through its public meetings and requests for information—on topics related to payment models and to report its findings to the Department of Health and Human Services. Source: PTAC and Centers for Medicare & Medicaid Services. | GAO‑26‑107953 |
Idea and concept. The Innovation Center identifies ideas for health care payment and delivery approaches that may be tested in a model from across the agency, other federal agencies, and from external sources.[15] For instance, the Innovation Center may solicit ideas from experts across the health care field through listening sessions and requests for information. In addition, the Innovation Center has considered model ideas recommended by the Physician-Focused Payment Model Technical Advisory Committee (PTAC), based on proposals submitted by stakeholders, such as physicians, provider associations, and health systems.[16]
The Innovation Center reviews ideas to determine if they may be developed into proposed models. Specifically, the Innovation Center assesses these model concepts in the context of its current portfolio of models as well as CMS and administration priorities.
Planning and design. The Innovation Center develops a model proposal that outlines the model design and evaluation plan as well as the potential effects of models. Specifically, proposals summarize supporting evidence and outline size and scope of a model; proposed research questions and measures; an implementation plan, including how participants will be selected; and the model’s potential effect on cost and quality. In addition, the Office of the Actuary estimates the likely effect on federal spending for each proposed model, according to Office of the Actuary officials. According to these officials, there is a great deal of uncertainty in these initial projections because, for instance, there may be limited existing research on the potential effects of a model.
The Innovation Center considers multiple factors when determining if a proposal should be tested. These factors may include feasibility—including the likelihood it can be successfully operated and the potential it can be scaled beyond the test—and potential effect on health and federal savings. Once proposals receive approval from CMS, HHS, and the Office of Management and Budget, the Innovation Center can begin preparations to test the model.
Solicit and build. The Innovation Center builds the infrastructure needed to operate and evaluate the model. The Innovation Center estimates that this part of the process typically takes between 18 and 36 months to complete. The Innovation Center and its contractors will develop information technology systems (for instance to collect data necessary to monitor the model), develop learning supports for participants, and finalize an evaluation plan.
The Innovation Center also solicits, selects, and establishes agreements with model participants, such as health care provider organizations or states.[17] The requirements that the Innovation Center sets for participants vary by model. For example, participants may be required to have certain organizational capacities, like the availability of electronic health records. In addition, the participants may be selected to achieve a balance of characteristics for evaluation purposes, like geographic location. The nature of participation also varies by model. Models may have voluntary participation—meaning participants choose to join the model—or mandatory participation—meaning participants are required to join the model.
Operate and evaluate. The Innovation Center operates models for a defined testing period and evaluates the effects of the model on federal spending and health care quality. The model testing period is determined by the Innovation Center and has typically been less than 10 years, according to CMS. The Innovation Center monitors models, including annually reviewing model results to determine if the agency should make changes to the model, expand the model, or terminate it.
Model Expansion
Based on model results, CMS may expand the duration and scope of Innovation Center models if the following conditions are met:
· The agency determines that the expansion is expected to reduce spending without reducing the quality of care, or to improve quality without increasing spending.
· The agency determines that the expansion would not deny or limit coverage or benefits for beneficiaries.
· CMS’s Office of the Actuary certifies that the expansion will reduce or not increase net program spending.
To determine whether to certify a model for expansion, the Office of the Actuary assesses the likelihood that an expanded model would reduce federal spending, according to Office of the Actuary officials. To estimate an expanded model’s likely effect on federal spending, the Office of the Actuary reviews model evaluations from the testing period as well as other evidence and considers differences between the tested model and the potential expansion, according to officials.[18] For instance, when expanding a model, there may be differences in the characteristics of the participants or beneficiaries. Office of the Actuary officials told us that a model would be certified for expansion if they estimate there is a 90 to 95 percent likelihood the model would reduce federal spending.
Innovation Center Obligated $11.4 Billion and Operated 70 Models Testing Payment and Delivery Approaches
Innovation Center Obligated $11.4 Billion from Fiscal Years 2011 Through 2024
Innovation Center obligations totaled $11.4 billion from fiscal years 2011 through 2024, according to CMS obligations data.[19] These obligations come from the $20 billion that PPACA appropriated to the Innovation Center during this time period.[20] Specifically, the Innovation Center obligated $7.9 billion of its first $10 billion appropriation for fiscal years 2011 through 2019 and $3.5 billion in fiscal years 2020 through 2024, after receiving its second $10 billion appropriation for fiscal years 2020 through 2029.[21] Because these appropriated funds remain available until expended, $8.0 billion remained unobligated as of the end of fiscal year 2024.
Total annual obligations peaked at $1.3 billion in fiscal year 2015. Annual obligations have since decreased by nearly 40 percent to $789 million in fiscal year 2024. (See fig. 2.)
Figure 2: Center for Medicare and Medicaid Innovation (Innovation Center) Obligations, by Year and Category, Fiscal Years 2011–2024
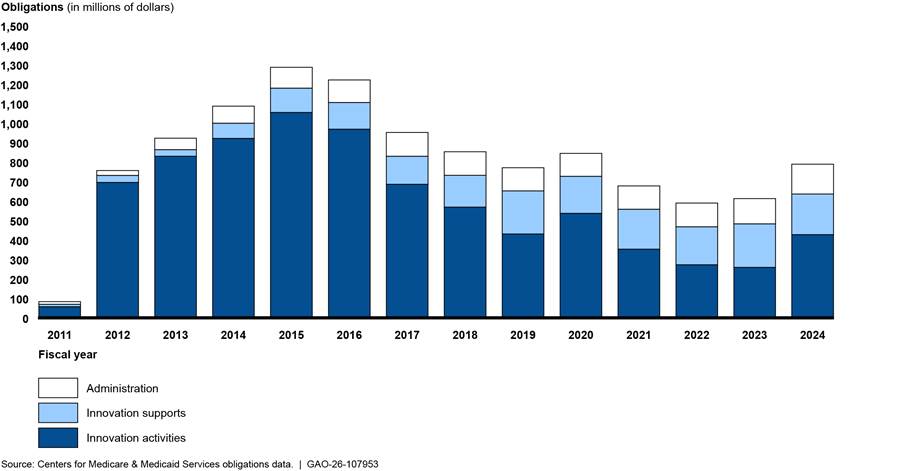
Note: Innovation activities include obligations that can be directly attributed to a specific model. Innovation supports include obligations that support the development or operation of multiple models. Administration includes payroll expenses and non-payroll administrative costs.
|
Center for Medicare and Medicaid Innovation (Innovation Center) Obligations Categories According to CMS officials, the Innovation Center’s obligations fall into three categories: innovation activities, innovation supports, and administration. Innovation activities include obligations that can be directly attributed to a specific model or initiative—such as contracts for implementation, monitoring, or evaluation and model payments to participants. Innovation supports include obligations that support the development or operation of multiple models, such as information technology. Administration includes payroll expenses and non-payroll administrative costs. Source: Centers for Medicare & Medicaid Services (CMS) . | GAO‑26‑107953 |
The decrease in total annual obligations since fiscal year 2015 was driven by a decrease in obligations toward model-specific innovation activities.[22] Innovation activities have represented the largest share of the Innovation Center’s annual obligations. Since fiscal year 2015, obligations for innovation activities have generally decreased—both in total and as a share of all obligations. Specifically, annual obligations for innovation activities decreased from over $1 billion (or 82 percent of obligations) in fiscal year 2015 to $427 million (or 54 percent of obligations) in fiscal year 2024.
According to CMS officials, the decrease in Innovation Center obligations since fiscal year 2015 reflects a leveling off in the number of models the Innovation Center operates as well as changes in how certain activities are tracked and reported.[23] Specifically, the Innovation Center has centralized common model functions to be more cost efficient, according to officials. For example, officials noted that the agency created centralized resources to support certain activities—like information technology and quality measure development—which simplified contract administration. These activities were thus recategorized from model-specific activities included under innovation activities to common innovation supports.
While total obligations have decreased, obligations for innovation supports (that spanned multiple models) and administration have increased—both in total and as a share of all obligations—since fiscal year 2015. Specifically, the annual obligations for innovation supports increased from $124 million (or 10 percent of obligations) in fiscal year 2015 to $209 million (or 27 percent of obligations) in fiscal year 2024. Obligations for administration increased from $108 million (or 8 percent of obligations) in fiscal year 2015 to $153 million (or 19 percent of obligations) in fiscal year 2024.
The Innovation Center Operated 70 Models Testing Payment and Delivery Approaches That Engaged a Range of Providers and Other Participants
As of January 2025, the Innovation Center had tested 70 models, ranging from six in 2011 to 31 in 2016. (See fig. 3.) The Innovation Center had concluded the testing of 46 of these models and was actively testing 24 models—referred to in this report as “active models.” (See app. 1 for details on the Innovation Center’s 70 models.)
Figure 3: Number of Annual Active and Cumulative Models Tested by the Center for Medicare and Medicaid Innovation (Innovation Center), 2011–January 2025
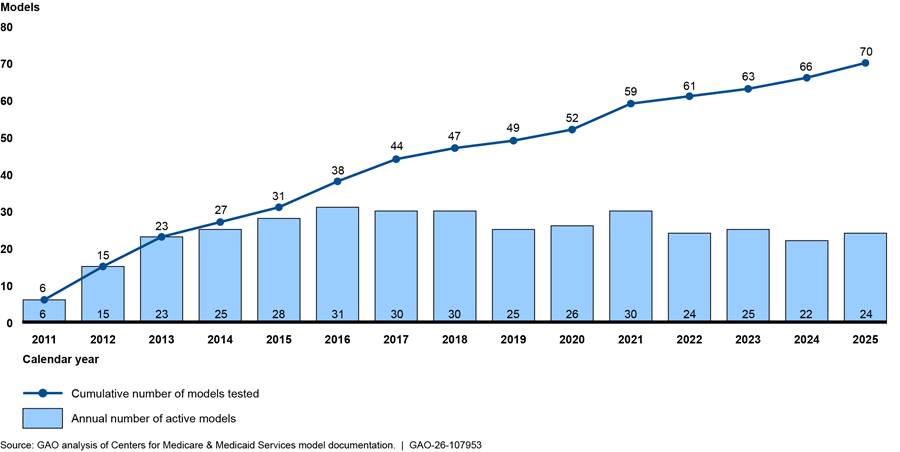
Note: The counts of models for 2011 through 2024 include models that were in operation at any point during the calendar year. The count of models for 2025 includes only those models that were in operation as of January 2025.
The 24 active models tested payment and delivery approaches with a range of focus areas, payment arrangements, and federal health programs. Specifically,
· Focus area. The Innovation Center sorted models into one or more categories based on the focus of each model. For example, there were nine models that focused on a specific disease or set of services (disease-specific or episode-based), including dementia, opioid misuse, and cancer.
· Payment arrangement. Models also varied by payment arrangement to participants. For instance, two models included bundled payments—a single payment for the cost of services provided during a defined episode of care—and five models included capitated payments—a set prepayment to cover predicted costs of all or some of the health care services for a specific patient over a certain period of time.
· Federal health program covered. Models also differed in terms of the programs covered, with 13 models covering Medicare only, four models covering Medicaid (two of which also covered CHIP), and seven models covering both Medicare and Medicaid.
See table 1 for a breakdown of active models across these selected characteristics as of January 2025. (Appendix I provides a full description of all 70 models tested by the Innovation Center).
|
Model Characteristics |
Description of models |
|
Focus areaa |
· Nine disease-specific and episode-based models, which aim to address deficits in care for a defined population with a shared specific disease or medical condition, procedure, or care episode · Nine accountable care models, in which accountable care organizations (ACO), hospitals, or other providers take financial responsibility for improving quality of careb · Nine state and community-based models, in which a state or community-based organization serves as the main participant · Three health plan models, which include Medicare Advantage plansc · Two statutory demonstrations, which have been required by law. Currently, both of these models focus on rural or critical access hospitals · One prescription drug model, which seeks to improve access to and the affordability of prescription drugs |
|
Payment arrangement to participantsa |
· 10 advanced alternative payment models, which are part of CMS’s Quality Payment Program and give incentive payments to reward high-quality care for participants that share in the financial rewards and risk of caring for beneficiaries · Five capitated payment models, in which providers receive a set prepayment to cover predicted costs of all or some of the health care services for a specific patient over a certain period of time · Two bundled payment models, in which providers receive a single payment for the combined cost of eligible services and supplies provided during a defined episode of care |
|
Federal program covered |
· 13 Medicare models · Four Medicaid models, two of which also covered the Children’s Health Insurance Program · Seven Medicare and Medicaid models |
Source: Centers for Medicare & Medicaid Services (CMS) model documentation. | GAO‑26‑107953
aA model may be included in more than one focus area or payment arrangement.
bAn ACO refers to a group of providers and suppliers of services, such as hospitals and physicians, that work together to coordinate care for the patients they serve.
cMedicare Advantage is the private plan alternative to Medicare fee-for-service.
In addition, these 24 active models included participants such as health care provider organizations, states, and others. Further, the nature of participation differed by model. Specifically, 22 models had voluntary participation and two had mandatory participation.
Most (16) of the 24 active models included health care provider organizations as participants. Participants in these models included many types of provider organizations, such as accountable care organizations (ACO)—in which a group of providers and suppliers of services, such as hospitals and physicians, work together to coordinate care—as well as hospitals; primary care practices; and specialized providers, like dialysis facilities. These models also reached different numbers of participants and providers.[24] For example, among the four models targeting ACOs, the number of participants ranged from one ACO with 3,721 providers to 103 ACOs with 136,665 providers, according to model data provided by CMS. (See table 2.)
|
Health care provider organization and model |
Number of participants |
Type of participant |
Number of providers affiliated with participants |
|
Accountable care organizations (ACO)a |
|
|
|
|
ACO REACH Modelb |
103 |
ACOs |
136,665 |
|
Kidney Care Choices Model |
94 |
Kidney contracting entities and kidney care first practicesc |
8,074 |
|
ACO Primary Care Flex Model |
24 |
ACOs |
18,538 |
|
Vermont All-Payer ACO Model |
1 |
ACO |
3,721 |
|
Hospitals |
|
|
|
|
Rural Community Hospital Demonstrationd |
20 |
Hospitals |
n/a |
|
Pennsylvania Rural Health Model |
18 |
Hospitals |
n/a |
|
Frontier Community Health Integration Project Demonstrationd |
5 |
Critical access hospitals |
n/a |
|
Hospitals and practices |
|
|
|
|
Maryland Total Cost of Care Model |
67 495 |
Hospitals Primary care practices |
6,170 |
|
Primary care practices |
|
|
|
|
Primary Care First Model |
1,810 |
Primary care practices |
12,225 |
|
Making Care Primary Model |
117 |
Primary care practices |
2,319 |
|
Specialized care providers |
|
|
|
|
Expanded Home Health Value-Based Purchasing Modele |
About 12,000 |
Home health agencies |
n/a |
|
End-Stage Renal Disease Treatment Choices Modele |
2,396 |
Dialysis facilities |
2,986 |
|
Medicare Diabetes Prevention Program Expanded Model |
928 |
Program suppliers including physicians, hospitals, community-based organizations, gyms, and other qualifying entities |
n/a |
|
Bundled Payments for Care Improvement Advanced Model |
42 128 |
Convenersf Non-convenersf |
7,313 |
|
Guiding an Improved Dementia Experience Model |
95 |
Dementia care program providers or suppliers |
1,399 |
|
Enhancing Oncology Model |
37 2 |
Oncology practices Commercial payers |
2,813 |
Legend: n/a = not applicable
Source: Centers for Medicare & Medicaid Services (CMS). | GAO‑26‑107953
Notes: Models included are those active as of January 2025 with health care provider organization participants. Participation data are current as of January to February 2025. Participants are entities that have a direct contractual relationship with CMS to implement the model, and providers are typically Medicare-enrolled providers and suppliers, such as individual clinicians, that engage in models through the participant, according to CMS officials.
aAn ACO refers to a group of providers and suppliers of services, such as hospitals and physicians, that work together to coordinate care for the patients they serve.
bACO REACH was previously called ACO Realizing Equity, Access, and Community Health.
cA kidney contracting entity includes nephrologists or nephrology practices and transplant providers and may include dialysis facilities and other providers and suppliers.
dStatutorily required model.
eModel has mandatory participation.
fA convener facilitates coordination among multiple entities and bears risk on behalf of those entities, while a non-convener only bears financial risk for itself. In this model, conveners include physician group practices (16), home health agencies (13), health systems (5), and other organizations (8). Non-conveners in this model include physician group practices (70) and acute care hospitals (58).
According to CMS officials, the Innovation Center has made a concerted effort to include more provider organizations that are safety-net providers that serve primarily low-income people and typically did not participate in early Innovation Center models. For example, the ACO Primary Care Flex Model targeted low-revenue ACOs, which tend to be made up of physicians and might include federally qualified health centers or serve rural areas. The model also strengthened incentives for providers to form ACOs in underserved areas.
Seven of the 24 active models included state participants. In these models, state participants included hospitals and other providers, drug manufacturers, and payers (e.g., health plans) as partners or as downstream participants.[25] For example, states participating in the Innovation in Behavioral Health Model recruited specialty behavioral health practices as participants. (See table 3.)
|
Model |
Number of states |
Other participants |
|
Cell and Gene Therapy Access Modela |
35 |
States work with two drug manufacturers of gene therapies for the treatment of sickle cell disease. |
|
Transforming Maternal Health Model |
15 |
States may partner with managed care organizations, hospitals, birth centers, health centers and rural health clinics, maternity care providers, and community-based organizations. |
|
Financial Alignment Initiative for Medicare-Medicaid Enrollees |
9 |
States participating in the capitated model option may partner with health plans.b |
|
Integrated Care for Kids Model |
6 |
States partner with hospitals or health systems (5), a mental health care provider (1), or a local health department (1).c |
|
Maternal Opioid Misuse Model |
7 |
States partner with hospitals or health systems (6) and a managed care organization (1). |
|
Innovation in Behavioral Health Model |
4 |
States recruit specialty behavioral health practices, including community mental health centers, opioid treatment programs, and public or private practices. |
|
Achieving Healthcare Efficiency Through Accountable Design Modeld |
3 |
States recruit hospitals and primary care practices. |
Source: Centers for Medicare & Medicaid Services (CMS). | GAO‑26‑107953
Note: Models included are those active as of January 2025 with state participants. Participation data are current as of January to February 2025 unless otherwise noted.
aState participation as of July 2025. The count of states includes the District of Columbia and Puerto Rico. CMS maintains the model arrangement directly with the two drug manufacturers.
bEight states operate a capitated model in which a health plan receives a prospective blended payment to provide comprehensive, coordinated care. One state operates a managed fee-for-service model in which the state is eligible to benefit from savings resulting from initiatives designed to improve quality and reduce costs for both Medicare and Medicaid.
cIn total, seven models operated across six states.
dAlso called the AHEAD Model. This model was previously called States Advancing All-Payer Health Equity Approaches and Development Model.
Finally, one of the 24 models included payers as the sole participant type.[26] The Medicare Advantage Value-Based Insurance Design Model included 62 Medicare Advantage organizations as participants.
CMS Certified Four Models for Expansion and Applied Lessons Learned; Agency Also Identified Factors That Affect Savings Potential
Four Certified Models Were Expected to Produce Savings and CMS Applied Lessons Learned from Successful Model Elements
The primary outcome of model testing is CMS’s decision on whether to certify each model for expansion—something CMS has done for four of the 70 models tested as of January 2025. These four models achieved net savings during the testing period. Based on its analysis, which includes the testing period results and other factors, the CMS Chief Actuary certified that, if expanded, the models were expected to reduce federal spending and thereby produce savings.[27] CMS also determined these models would maintain or improve patient care without limiting coverage or benefits. CMS has expanded four models through rulemaking or notice. In two cases, it launched a new nationwide version of the tested model within the Innovation Center. In two other cases, CMS incorporated the expanded model into other CMS programs. (See table 4.)
|
Model and years tested |
Delivery or payment approach tested |
Amount saved during testing |
Implementation after certification (implementation year) |
|
Pioneer Accountable Care Organization Model (2012-2016) |
Offer experienced accountable care organization providers more responsibility for costs and potential savings |
$384 million in Medicare savings in first 2 years |
Elements incorporated into another CMS program—Medicare Shared Savings Program (2015) |
|
Medicare Diabetes Prevention Programa (2012-2015) |
Provide coaching for Medicare beneficiaries with prediabetes, facilitating lifestyle changes and weight loss |
$2,650 saved per beneficiary during first 15 months of testing |
Expanded model within Innovation Center portfolio as the Medicare Diabetes Prevention Program Expanded Model (2018) |
|
Repetitive Scheduled Non-Emergent Ambulance Transport Model (Prior Authorization) (2014-2020) |
Require prior approval before Medicare pays for repeated, non-emergency ambulance rides (e.g., for dialysis) |
$1 billion in Medicare savings over 5 years |
Expanded model into other CMS programs—Medicare Fee-for-Service Compliance Programs (2020) |
|
Home Health Value-Based Purchasing Model (2016-2020) |
Reward home health providers that offer improved care, based on factors such as hospitalizations and quality outcomes |
$949 million in Medicare savings from 2016-2020 |
Expanded model within Innovation Center portfolio as the Expanded Home Health Value-Based Purchasing Model (2022) |
Source: Centers for Medicare & Medicaid Services (CMS). | GAO‑26‑107953
Note: Three of the four models—Pioneer Accountable Care Organization Model, Medicare Diabetes Prevention Program, and Repetitive Scheduled Non-Emergent Ambulance Transport Model (Prior Authorization)—were voluntary, meaning participants chose to join the model. The Home Health Value-Based Purchasing Model was mandatory.
aThe Medicare Diabetes Prevention Program was part of the Innovation Center’s Health Care Innovation Awards Round One Model, which funded awardees to test payment and delivery approaches.
In the Innovation Center’s 2024 report to Congress and other sources, CMS has reported on its ability to expand models on the basis of quality improvements. Specifically, CMS has reported that it has not expanded any models primarily based on quality improvements, although it may do so by law if the model does not increase spending. The model testing process assessed quality improvement, as required by statute, but the agency has reported that models designed in the Innovation Center’s first decade focused on decreasing spending—rather than improving quality—as their primary aim.[28] Further, CMS has reported that model evaluations typically focused on claims-based quality indicators, which offered information about what services were provided—often targeting a reduction in avoidable services—but which have limited information about any quality improvements related to patient experience. As of 2024, CMS reported developing a new strategy to enhance its ability to expand models primarily on the basis of quality improvements. For example, the agency indicated that the model development and evaluation processes now include earlier identification of quality goals and expanded use of patient-reported quality measures, to inform model evaluation methods.
In addition to expanding models, the Innovation Center may also identify promising model elements that it may then incorporate into new models for further testing—known as successor models—or incorporate into Medicare programs.
· Develop successor models. To build upon elements of prior models, the Innovation Center has tested successor models that make progress toward possible expansion through multiple iterations of a concept. As of January 2025, the Innovation Center was testing nine successor models included among the 24 active models.[29] The Innovation Center continues to develop successor models, including two new models.[30] A successor model may represent a direct follow-on to an individual model. For example, the Bundled Payments for Care Improvement Advanced Model refines prior models—the Bundled Payments for Care Improvement Models—with features such as a streamlined model design that ties payment to quality measures. Alternately, a successor model may instead build upon elements of models related by disease category or payment method. For example, the Increasing Organ Transplant Access Model shares a focus on kidney disease with two prior models, Kidney Care Choices and End-Stage Renal Disease Treatment Choices and builds upon the prior models’ use of direct financial incentives to increase the number of kidney transplants, but specifically focuses on transplant hospitals.[31]
· Incorporate into Medicare programs. Outside of the formal expansion process, CMS has formalized successful model elements as permanent features of Medicare. For example, CMS incorporated an element of the ACO Investment Model—providing rural or small ACOs with up-front payments to invest in infrastructure and staffing—into the Medicare Shared Savings Program in 2023.[32] CMS also incorporated an element of Partnership for Patients—providing hospitals with technical assistance in implementing best practices for reducing preventable patient harm and hospital readmissions—into its Quality Improvement Organization program.
In addition to building upon successful model elements, the Innovation Center produces and distributes knowledge generated from the model testing process. It conducts this outreach through webinars and blog posts targeting audiences such as providers, beneficiary groups, and researchers. For example, the Innovation Center encouraged health care providers to adopt a screening tool for health-related social needs developed in the Accountable Health Communities Model by making it publicly available for providers.
CMS Has Identified Factors That Affect the Potential for Models to Generate Savings
The Innovation Center has identified factors that affect the potential for models to generate savings during testing, including incentive payments to participants, selection bias, and participant attrition, which are all factors associated with voluntary models.
· Incentive payments. Voluntary models often employ generous financial incentive payments to ensure robust participation, but these payments may make it difficult for models to demonstrate net savings during the testing period.
· Selection bias. Voluntary models make savings difficult to achieve because they often produce selection bias, meaning that participants may only join models in which they anticipate generating financial savings, thus qualifying for shared savings or bonus payments.
· Participant attrition. Participants in voluntary models may end their participation when facing possible financial losses. In such scenarios, participants often leave before the model has the opportunity to realize savings. (See text box.)
|
Participant Attrition in Center for Medicare and Medicaid Innovation (Innovation Center) Models · Participant attrition varies greatly across models. Specifically, participant attrition among health care provider organizations ranged from zero to 78 percent among the 18 models that had completed testing and had final evaluations. · Model evaluations reported participants’ stated reasons for leaving these models. Common reasons included o financial losses or the prospect of assuming financial risk; o administrative burden; o organizational changes (such as leadership changes or mergers); o shifting participation to another model or value-based payment arrangement, such as accountable care organizations within the Medicare Shared Savings Program; and o unable to meet model criteria (e.g., serving a minimum number of Medicare beneficiaries) for participation. · In addition, several model evaluations noted that participants that dropped out tended to be smaller in size. · According to CMS officials, the agency has tried to address participant attrition through various strategies. For instance, strategies have included implementing more predictable payment mechanisms, streamlining reporting requirements, and offering technical assistance. Source: GAO analysis of model evaluations and interviews with Centers for Medicare & Medicaid Services (CMS) officials. | GAO‑26‑107953 |
Most models tested have been voluntary. Officials told us voluntary models may be appropriate when new payment approaches are not sufficiently tested to support implementation in a mandatory model or where the Innovation Center has confidence that a voluntary model will not experience selection bias. However, voluntary models may make it more difficult to reduce spending during the testing period because payment approaches must be designed to attract participants. It is also challenging to expand a voluntary model into a mandatory model because of difficulties predicting future savings, according to officials. While the Innovation Center was testing two mandatory models out of 24 active models in January 2025, it plans to increase the proportion of mandatory models in its portfolio, according to officials. For example, the Innovation Center began testing the mandatory Increasing Organ Transplant Access Model in July 2025 and the mandatory Transforming Episode Accountability Model in January 2026. It plans to begin testing the mandatory Ambulatory Specialty Model in January 2027.
Additionally, the typical model test duration of less than 10 years may make federal savings difficult to achieve. CMS has noted that models that focus on primary care may require longer testing periods to demonstrate savings, as their emphasis on preventive care often takes time to observe changes. Providers participating in primary care models may require additional time to invest in care coordination staffing and health information technology, which could also extend the test duration necessary to reduce spending.
The Innovation Center Established Goals and Performance Measures with Targets
The Innovation Center uses selected performance management practices to regularly assess the performance of its efforts to test the effects of new health care delivery and payment approaches, ultimately supporting its mandate to reduce federal health care spending and improve quality of care. These selected performance management practices include establishing long-term and near-term goals, as well as using performance information to assess evidence.
|
Selected Practices for Performance Management Performance management practices define what an agency is trying to achieve, determine how well programs are performing, and identify how to improve results. These practices include the following: · Establishing long-term goals, which are the desired outcomes for the agency’s program and set a general direction for a program’s efforts. To ensure progress can be assessed, each long-term goal is broken down into one or more near-term goals. · Establishing near-term goals, which define the specific results a program is expected to achieve in the near-term. They align with an agency’s long-term goals and include performance measures—quantitative targets and time frames against which to track the progress of agency efforts. Agencies collect evidence, such as performance measures, to measure actual performance toward results. · Using performance information, which allows an agency to regularly assess evidence to inform decisions and ensure further progress toward achieving goals. Source: GAO. | GAO‑26‑107953 |
In May 2025, the Innovation Center established new long-term goals to outline the agency’s vision for its activities (see table 5). These long-term goals will shape the Innovation Center’s portfolio of models, including by guiding the development of new models and by informing any decisions to alter or terminate active models, according to officials. To support these goals, the Innovation Center also identified a foundational principle—protecting federal taxpayers—in line with its mandate to reduce federal spending and improve quality of care. Additionally, the Innovation Center developed near-term goals, including performance measures with targets and time frames, to accompany the May 2025 long-term goals. (See table 5.)
Table 5: Center for Medicare and Medicaid Innovation (Innovation Center) Long-Term Goals and Examples of Related Near-Term Goals and Performance Measures, as of December 2025
|
Long-Term goals |
Near-Term goals (examples) |
Performance measures (examples) |
|
Promoting evidence-based prevention - incentivize preventive care and health promotion to help people avoid illness and optimally manage chronic disease. |
Increase weighting of outcomes measures across Centers for Medicare & Medicaid Services’s value-based programs. |
Share of measures across models that are outcome-based. 2025 baseline: 52% 2026 target: 53% |
|
Empowering people to achieve their health goals - feature tools, information, and processes that better connect people to their health data and empower them to make informed health decisions. |
Increase the percent of models that promote health data management tools, shared decision-making guides, tracking technology, or artificial intelligence health guides. |
Share of models that promote health data management tools. 2025 baseline: 10% 2026 target: 30% |
|
Driving choice and competition - test models and features aimed at promoting competition in health care markets. |
Maintain or increase the share of accountable care organizations (ACO) and providers under two-sided risk arrangements and reduce benchmark arbitrage in ACO programs.a,b,c,d |
Percent of original Medicare beneficiaries in a two-sided risk arrangement, including those in Innovation Center models. 2025 baseline: 40% 2026 target: 45% |
Source: Centers for Medicare & Medicaid Services (CMS). | GAO‑26‑107953
aThis near-term goal also applies to the Innovation Center’s foundational principle—protecting federal taxpayers—that is associated with these long-term goals.
bAn ACO refers to a group of providers and suppliers of services, such as hospitals and physicians, that work together to coordinate care for the patients they serve.
cTwo-sided risk arrangements include both upside and downside risk in which participants who deliver quality care at a lower cost may be eligible to receive a payment from CMS, while participants who increase overall spending may owe a payment to CMS.
dBenchmarks are spending targets against which CMS measures ACO financial performance and, ultimately, eligibility for an additional payment based on shared savings between CMS and the ACO. An ACO may have the opportunity for arbitrage if it is able to achieve favorable performance relative to the benchmark without improving efficiency. For example, ACOs can improve their financial performance by dropping high-spending practices or practices with sicker patients; this would result in lower spending for the ACO without an improvement in efficiency.
According to officials, the Innovation Center began assessing the outcomes of its activities against these near-term goals in the summer of 2025. It plans to use the performance information obtained through these regular assessments internally to track progress against the Innovation Center’s long-term goals, according to officials.
Agency Comments
We provided a draft of this report to HHS for review and comment. HHS provided technical comments, which we incorporated as appropriate.
We are sending copies of this report to the appropriate congressional committees, the Secretary of Health and Human Services, the Administrator of CMS, and other interested parties. In addition, the report will be available at no charge on GAO’s website at http://www.gao.gov.
If you or your staff have any questions about this report, please contact me at GordonLV@gao.gov. Contact points for our Offices of Congressional Relations and Media Relations may be found on the last page of this report. Other major contributors to this report are listed in appendix II.
Sincerely,

Leslie V. Gordon
Director, Health Care
As of January 2025, the Innovation Center was actively testing 24 models and had concluded the testing of 46 models. Tables 6 and 7 describe these models, when they were tested, how the Innovation Center categorized them, and obligations for these models.
Table 6: Active Models Tested by the Center for Medicare and Medicaid Innovation (Innovation Center), as of January 2025
|
Model name and description |
Calendar years tested |
Focus area(s) |
Obligations, fiscal years 2011–2024a (in millions) |
|
Accountable Care Organization (ACO) Primary Care Flex Model – tests the effectiveness of prospective payments and increased funding for primary care in ACOs to impact health outcomes as well as the quality and cost of care.b This model aims to increase the number of low-revenue ACOs in the Medicare Shared Savings Program. |
2025–2029 |
· Accountable care models |
$14 |
|
ACO REACH Model – tests higher and lower risk-sharing options with either primary care or total care capitation for provider-led ACOs managing Medicare fee-for-service beneficiaries. This model offers tracks for ACOs predominantly serving high-need populations and newer ACOs. This model was previously called ACO Realizing Equity, Access, and Community Health. |
2023–2026 |
· Accountable care models |
$142c |
|
Achieving Healthcare Efficiency Through Accountable Design Model – tests a state-based total cost of care approach whereby participating states will assume responsibility for managing the cost and quality across all payers, including Medicare, Medicaid, and private coverage. Participating states receive funding and targeted support from CMS to develop and implement strategies to improve quality and reduce costs including hospital global budgets, advanced primary care, multi-payer alignment, and investments in population health activities. Also called the AHEAD Model. This model was previously called States Advancing All-Payer Health Equity Approaches and Development. |
2024–2034 |
· State & community-based models |
$21 |
|
Bundled Payments for Care Improvement Advanced Model – tests a bundled payment approach where the participating hospitals and practices are responsible for the quality and total cost of care during a clinical episode (from hospital admission or outpatient procedure through 90 days after discharge or the procedure). |
2018–2025 |
· Disease-specific & episode-based models |
$115 |
|
Cell and Gene Therapy Access Model – tests outcomes-based agreements, negotiated by CMS on behalf of states, for cell and gene therapies. This model initially aims to increase access to treatments for Medicaid beneficiaries living with sickle cell disease. |
2025–tbdd |
· Prescription drug models |
$15 |
|
End-Stage Renal Disease Treatment Choices Model – tests payment adjustments for dialysis facilities and use of patient education to encourage greater use of home dialysis and kidney transplants for Medicare beneficiaries with end-stage renal disease. This model has mandatory participation. |
2021–2025 |
· Disease-specific & episode-based models |
$31 |
|
Enhancing Oncology Model – tests a bundled payment for oncology practices to take accountability for episodes of care surrounding cancer treatment. This model focuses on oncology care coordination for Medicare fee-for-service beneficiaries with certain common cancer types. |
2023–2030 |
· Disease-specific & episode-based models · Accountable care models |
$21 |
|
Expanded Home Health Value-Based Purchasing Model – tests the effectiveness of tying payments for Medicare-certified home health agencies to the quality of care provided. This model expanded the Home Health Value-Based Purchasing Model to all fifty states, District of Columbia, and the U.S. territories. This model has mandatory participation. |
2022–tbd |
· Disease-specific & episode-based models |
$58e |
|
Financial Alignment Initiative for Medicare-Medicaid Enrollees – tests improved financial alignment between Medicare and Medicaid to improve care coordination for beneficiaries in both programs. Participating states may choose (1) the capitated model—in which health plans receive an upfront payment to provide care; or (2) the managed fee-for-service model—in which states are eligible to share in savings from initiatives designed to improve quality and reduce costs for Medicare and Medicaid. |
2013–2025 |
· State & community-based models · Health plan models |
$292 |
|
Frontier Community Health Integration Project Demonstration – tests strategies to encourage critical access hospitals to provide essential services in rural communities to increase access to care for Medicare beneficiaries living in rural communities. |
2016–2019, 2022–2027 |
· Statutory demonstrations and other projects |
n/a |
|
Guiding an Improved Dementia Experience Model – tests an alternative payment methodology for the delivery of dementia care. This model requires participants to provide comprehensive care coordination and care management to Medicare beneficiaries with dementia, caregiver education and support, and respite-like services to beneficiaries with dementia in certain situations. |
2024–2032 |
· Disease-specific & episode-based models |
$27 |
|
Innovation in Behavioral Health Model – tests monthly care management and performance-based payments to behavioral health providers that deliver integrated care across behavioral, physical, and social needs for beneficiaries of Medicare or Medicaid with mental health conditions or substance use disorders. |
2025–2032 |
· State & community-based models |
$6 |
|
Integrated Care for Kids Model – tests state-designed alternative payment models for children covered by Medicaid and the Children’s Health Insurance Program (CHIP). This model encourages prevention, early identification, and treatment of behavioral and physical health needs. |
2020–2026 |
· State & community-based models |
$116 |
|
Kidney Care Choices Model – tests risk-based payment arrangements to hold kidney care focused ACOs responsible for the cost and quality of Medicare patients who have late-stage chronic kidney disease, end-stage renal disease, or a kidney transplant. |
2022–2027 |
· Accountable care models · Disease-specific & episode-based models |
$103 |
|
Making Care Primary Model – tests strategies to enable primary care clinicians with varying levels of experience in value-based care to gradually adopt prospective, population-based payments while building infrastructure to improve behavioral health and specialty integration and increase access to care. |
2024–2025 |
· Accountable care models |
$32 |
|
Maryland Total Cost of Care Model – tests a capitated payment for the total cost of care, which holds the state fully accountable for Medicare beneficiaries in Maryland. This model aims to improve the overall health of Marylanders and reduce avoidable hospital readmissions and emergency department visits. |
2019–2025 |
· State & community-based models · Accountable care models |
$74 |
|
Maternal Opioid Misuse Model – tests state-specific approaches to integrating maternal physical and behavioral health with treatment for opioid use disorder. This model aims to improve the quality of care for pregnant and postpartum women and their infants while also reducing overall associated Medicaid costs. |
2020–2025 |
· State & community-based models · Disease-specific & episode-based models |
$54 |
|
Medicare Advantage Value-Based Insurance Design Model – tests the effectiveness of offering Medicare Advantage plans the flexibility to design and offer reduced cost sharing or additional supplemental benefits to enrollees with chronic conditions with the goal of incentivizing beneficiaries to use high-value services. |
2017–2025 |
· Health plan models · Disease-specific & episode-based models |
$50 |
|
Medicare Diabetes Prevention Program Expanded Model – tests the effectiveness of an evidence-based intervention targeted to prevent the onset of type 2 diabetes among Medicare beneficiaries with an indication of prediabetes. This model expanded the Medicare Diabetes Prevention Program that was part of the Health Care Innovation Awards Round One model. |
2018–tbd |
· Disease-specific & episode-based models · Health plan models |
$22 |
|
Pennsylvania Rural Health Model – tests use of fixed upfront payments for participating rural hospitals enabling them to redesign care delivery to improve quality of care and meet the needs of their local communities. |
2019–2026 |
· State & community-based models · Accountable care models |
$29 |
|
Primary Care First Model – tests payment arrangements including upside and downside financial risk to hold participants responsible for care and to support the delivery of advanced primary care. Participants must take a patient-centered approach to care through features such as 24 hours a day, 7 days a week clinician access. |
2021–2025 |
· Accountable care models |
$149 |
|
Rural Community Hospital Demonstration – tests the provision of higher Medicare payments for covered inpatient hospital services to support participating small rural community hospitals—that are too large to be critical access hospitals—to meet the needs of people with Medicare. |
2004–2028 |
· Statutory demonstrations and other projects |
n/a |
|
Transforming Maternal Health Model – tests state strategies to improve health outcomes, safety, and overall patient experiences for mothers and their newborns in Medicaid and CHIP, while also reducing total program expenditures. This model provides technical assistance support to state Medicaid agencies and providers, including those in rural and other high-need areas, and financial incentives to participating state Medicaid agencies. |
2025–2034 |
· State & community-based models |
$8 |
|
Vermont All-Payer ACO Model – tests whether an ACO aligned across Medicare, Medicaid, and commercial insurance will incentivize broad delivery system transformation to reduce statewide spending and improve population health outcomes. The model establishes state and ACO-level accountability for health outcomes. |
2017–2025 |
· State & community-based models · Accountable care models |
$36 |
Legend: n/a = not applicable; tbd = to be determined
Source: Centers for Medicare & Medicaid Services (CMS) documentation. | GAO 26-107953
aObligated amounts reflect commitments to participants in the testing of models, such as health care providers of services, states, conveners, and others. These commitments may include care management fees and cooperative agreement awards and are paid through Innovation Center funds as appropriated under section 1115A of the Social Security Act. Some statutory models are not funded through section 1115A obligations.
bAn ACO refers to a group of providers and suppliers of services, such as hospitals and physicians, that work together to coordinate care for the patients they serve.
cAmount includes obligations for both the ACO REACH Model and its predecessor model (Global and Professional Direct Contracting Model).
dThis model started between January 1, 2025, and January 1, 2026, and will be tested for up to approximately 11 years, depending on the state.
eAmount includes obligations for both the Expanded Home Health Value-Based Purchasing Model and its predecessor model (Home Health Value-Based Purchasing Model).
Table 7: Completed Models Tested by the Center for Medicare and Medicaid Innovation (Innovation Center), 2011–2024
|
Calendar years tested |
Focus area(s) |
Obligations, fiscal years 2011–2024a (in millions) |
|
|
Accountable Care Organization (ACO) Investment Model – tested the effectiveness of prepaid shared savings in encouraging new Medicare Shared Savings Program ACOs to form in rural and underserved areas and in encouraging current Medicare Shared Savings Program ACOs to transition to arrangements with greater financial risk.b |
2015–2018 |
· Accountable care models |
$110 |
|
ACO Track 1 Plus Model – tested the effectiveness of offering an advanced alternative payment model with a more limited risk track than what was available in the Medicare Shared Savings Program to encourage more Medicare Shared Savings Program ACOs, especially ACOs composed solely of small physician practices and small rural hospitals, to take on financial risk. |
2018–2021 |
· Accountable care models |
$30 |
|
Accountable Health Communities Model – tested the effectiveness of systematically identifying and addressing the health-related social needs of beneficiaries at reducing health care costs and utilization among Medicare and Medicaid beneficiaries. |
2017–2023 |
· State & community-based models |
$148 |
|
Advance Payment ACO Model – tested the effectiveness of providing physician-based and rural Medicare Shared Savings Program ACOs with upfront and monthly payments that they could use to invest in care coordination activities |
2012–2015 |
· Accountable care models |
$72 |
|
Bundled Payments for Care Improvement Model 1, Retrospective Acute Care Hospital Stay Only – tested the effectiveness of a payment arrangement for inpatient hospital stays of Medicare beneficiaries. In this model, hospitals received discounted payments and physicians were paid their standard rates. Hospitals were held financially responsible for the cost of all Medicare services provided 30 days after discharge that exceeded historical trends. |
2013–2016 |
· Disease-specific & episode-based models |
$105c |
|
Bundled Payments for Care Improvement Model 2, Retrospective Acute & Post-Acute Care Episode – tested the effectiveness of a payment arrangement in which acute care hospitals and physician group practices received additional payments or made recoupment payments if the total costs for Medicare services provided during an inpatient hospital stay and up to 90 days after discharge were over or under a predetermined target price. |
2013–2018 |
· Disease-specific & episode-based models |
$105c |
|
Bundled Payments for Care Improvement Model 3, Retrospective Post-Acute Care Only – tested the effectiveness of a payment arrangement in which post-acute care providers—such as a skilled nursing facility, inpatient rehabilitation facility, long-term care hospital or home health agency—or physician group practices received payments or made recoupment payments if total costs for certain Medicare services were over or under a predetermined target price. These services were those provided during a clinical episode beginning with post-acute care services and included all services up to 90 days after the hospital discharge that preceded the post-acute care services. |
2013–2018 |
· Disease-specific & episode-based models |
$105c |
|
Bundled Payments for Care Improvement Model 4, Prospective Acute Care Hospital Stay Only – tested the effectiveness of making a single, predetermined payment in advance for all Medicare services furnished by a hospital, physicians, and other practitioners during an inpatient stay in an acute care hospital. Physicians and other practitioners submitted “no-pay” claims to Medicare and were paid by the hospital out of the advance bundled payment. |
2013–2018 |
· Disease-specific & episode-based models |
$105c |
|
Community-Based Care Transitions Program – tested approaches to reduce unnecessary hospital readmissions by improving the transition of Medicare beneficiaries from the inpatient hospital setting to home or to other care settings. |
2012–2017 |
· Statutory demonstrations and other projects · State & community-based models |
n/a |
|
Community Health Access and Rural Transformation Model – tested seed funding, payment structures, operational and regulatory flexibilities, and technical and learning support to empower rural communities to develop a high-quality care delivery system. |
2021–2023 |
· State & community-based models |
$9 |
|
Comprehensive Care for Joint Replacement Model – tested the effectiveness of a payment arrangement in which acute care hospitals received additional payments or made recoupment payments if the total costs for certain Medicare services were over or under a predetermined target price. These services were those provided during a clinical episode that includes an inpatient hospital stay related to a hip or knee replacement surgery and all services up to 90 days after discharge. |
2016–2024 |
· Disease-specific & episode-based models |
$79 |
|
Comprehensive End-Stage Renal Disease Care Model – tested the effectiveness of an ACO delivery and payment approach for providing care to end-stage renal disease beneficiaries. |
2015–2021 |
· Accountable care models · Disease-specific & episode-based models |
$111 |
|
Comprehensive Primary Care Initiative – tested the impact of enhanced primary care services, including care coordination, prevention, and 24-hour access. The initiative included multiple payers, and participating providers received a monthly care management fee and an opportunity to share in any net savings to the Medicare program. |
2013–2016 |
· Accountable care models |
$390 |
|
Comprehensive Primary Care Plus Model – tested the impact of enhanced primary care services for Medicare and Medicaid beneficiaries, including care coordination, prevention, and 24-hour access. The initiative included multiple payers, and participating providers received a monthly care management fee, performance-based incentive payments, and payments under the Medicare physician fee schedule. |
2017–2021 |
· Accountable care models |
$492 |
|
Emergency Triage, Treat, and Transport Model – tested approaches that provided greater ambulance care team flexibility to transport Medicare beneficiaries to alternative treatment sites following a 911 call. This model aimed to lower costs through a reduction in avoidable transports to an emergency department, and avoidable hospitalizations following those transports. |
2021–2023 |
· Disease-specific & episode-based models |
$32 |
|
Federally Qualified Health Center Advanced Primary Care Practice Demonstration – tested the effectiveness of paying a monthly care management fee for each eligible Medicare beneficiary receiving primary care services from federally qualified health centers to support team-led care, improved access and enhanced primary care services.d |
2011–2014 |
· Statutory demonstrations and other projects · Accountable care models |
$69 |
|
Global and Professional Direct Contracting Model – tested alternative approaches to risk-sharing arrangements and payments—with higher and lower risk-sharing options—for ACOs managing Medicare fee-for-service beneficiaries. |
2021–2022 |
· Accountable care models |
$142e |
|
Graduate Nurse Education Demonstration – tested the effect of offsetting the costs of clinical training for advanced practice registered nurses on the availability of graduate nursing students enrolled in training programs. |
2012–2018 |
· Statutory demonstrations and other projects |
n/a |
|
Health Care Innovation Awards Round One – provided funding to awardees, including providers, local government, and public-private partnerships, to test new care delivery and payment models for beneficiaries enrolled in Medicare, Medicaid, or the Children’s Health Insurance Program (CHIP). |
2012–2015 |
· Statutory demonstrations and other projects |
$1,290f |
|
Health Care Innovation Awards Round Two – provided funding to awardees to test new care delivery and payment models for beneficiaries enrolled in Medicare, Medicaid, or CHIP. |
2014–2017 |
· Statutory demonstrations and other projects |
$1,290f |
|
Home Health Value-Based Purchasing Model – tested the effectiveness of tying payments for Medicare-certified home health agencies to the quality of care provided. |
2016–2020 |
· Disease-specific & episode-based models |
$58g |
|
Hyperbaric Oxygen Therapy Model (Prior Authorization) – tested the effectiveness of prior authorization of non-emergent hyperbaric oxygen therapy. |
2015–2018 |
· Statutory demonstrations and other projects |
$5 |
|
Independence at Home Demonstration – tested the effectiveness of delivering an expanded scope of primary care services in a home setting on improving care for Medicare beneficiaries with multiple chronic conditions. |
2012–2023 |
· Statutory demonstrations and other projects |
n/a |
|
Initiative to Reduce Avoidable Hospitalizations Among Nursing Facility Residents: Phase One – tested effectiveness of partnerships between independent organizations and long-term care facilities to enhance onsite services to reduce hospitalizations for Medicare-Medicaid beneficiaries. |
2012–2016 |
· Disease-specific & episode-based models |
$239h |
|
Initiative to Reduce Avoidable Hospitalizations Among Nursing Facility Residents: Phase Two – tested whether a new payment model for a new set of long-term care facilities, as well as for long-term care facilities that participated in the initial phase of the model and continued to offer enhanced onsite services, would improve quality of care by reducing avoidable hospitalizations, while also lowering combined Medicare and Medicaid spending. |
2016–2020 |
· Disease-specific & episode-based models |
$239h |
|
Maryland All-Payer Model – tested the effectiveness of an all-payer system for hospital payment on quality of care and cost. |
2014–2018 |
· State & community-based models · Accountable care models |
$21 |
|
Medicaid Emergency Psychiatric Demonstration – tested whether reimbursing private psychiatric hospitals for certain psychiatric services for which Medicaid reimbursement has generally been unavailable would support higher quality care at a lower total cost. |
2012–2015 |
· Statutory demonstrations and other projects · Health plan models |
n/a |
|
Medicaid Incentives for the Prevention of Chronic Diseases Model – tested states providing incentives for Medicaid beneficiaries to participate in prevention programs and demonstrate changes in health risks and outcomes. |
2011–2015 |
· Statutory demonstrations and other projects |
n/a |
|
Medicare Care Choices Model – tested the effectiveness of providing Medicare beneficiaries the option to receive hospice-like support services from certain hospice providers while concurrently receiving curative services. |
2016–2021 |
· Disease-specific & episode-based models |
$27 |
|
Medicare Imaging Demonstration – tested whether the use of decision support systems could improve quality of care by promoting appropriate ordering of certain advanced imaging services. |
2011–2013 |
· Statutory demonstrations and other projects |
n/a |
|
Medicare Intravenous Immune Globulin Demonstration – tested the effectiveness of providing payment and items for services needed for in-home administration of intravenous immune globulin for the treatment of primary immunodeficiency disorders. |
2014–2023 |
· Statutory demonstrations and other projects |
n/a |
|
Million Hearts®: Cardiovascular Disease Risk Reduction Model – tested the effectiveness of providing financial incentives for health care providers to reduce the patients’ risk of heart attack and stroke on outcomes and accountability for costs among Medicare beneficiaries. |
2017–2021 |
· Disease-specific & episode-based models |
$50 |
|
Multi-Payer Advanced Primary Care Practice Demonstration – tested payment of care management fees to cover advanced primary care services provided by participants including care coordination and improved access. Participating states also included mechanisms to offer participating practices community support and linkages to states health promotion initiatives. |
2011–2016 |
· Statutory demonstrations and other projects · Accountable care models |
n/a |
|
Next Generation ACO Model – tested the effect of strong financial incentives for ACOs, coupled with tools to support better patient engagement and care management. Participating ACOs assumed higher levels of risk and reward than in other Centers for Medicare & Medicaid Services (CMS) ACO initiatives. |
2016–2021 |
· Accountable care models |
$131 |
|
Oncology Care Model – tested the effectiveness of a payment arrangement in which providers received a monthly payment for each Medicare beneficiary during a 6-month episode of care following the administration of chemotherapy and could earn additional performance-based payments if the total costs for Medicare services provided during the episode were under a predetermined target price. Starting in 2017, practices received higher performance-based payments by taking on risk for costs that exceed the target price. |
2016–2022 |
· Disease-specific & episode-based models |
$134 |
|
Part D Enhanced Medication Therapy Management Model – tested the effectiveness of providing certain Medicare prescription drug plans with the regulatory flexibility to design and implement innovative medication therapy management programs. The goal of the model was to optimize medication use. |
2017–2021 |
· Health plan models · Prescription drug models |
$38 |
|
Part D Payment Modernization Model – tested the impact of changes to prescription drug plan benefit design and payment structure on overall Medicare Part D expenditures and beneficiary out-of-pocket costs. |
2020–2021 |
· Prescription drug models |
$3 |
|
Part D Senior Savings Model – tested the effect of enhanced alternative Part D plan options that offered lower out-of-pocket costs for insulin as supplemental benefits. |
2021–2023 |
· Prescription drug models · Health plan models |
$9 |
|
Partnership for Patients – tested whether a coordinated, goal-directed, national collaborative approach for systematically spreading known best practices in patient safety could make acute care hospitals safer, more reliable, and less costly by reducing hospital acquired conditions and readmissions. |
2011–2016 |
· Disease-specific & episode-based models |
$561 |
|
Pioneer ACO Model – tested the effectiveness of allowing experienced ACOs to take on greater financial risk and reward than ACOs that participated in the Medicare Shared Savings Program. Participants that met certain levels of savings in the first two years were eligible to receive prospective per-beneficiary per-month payments. |
2012–2016 |
· Accountable care models |
$109 |
|
Repetitive Scheduled Non-Emergent Ambulance Transport Model (Prior Authorization) – tested the effectiveness of prior authorization for repetitive scheduled non-emergent ambulance transport. |
2014–2020 |
· Statutory demonstrations and other projects |
$38 |
|
State Innovation Models Initiative: Round One – tested the effectiveness of financial, technical, and other support to states that were either prepared to test or were committed to design and test new payment and service delivery models for beneficiaries enrolled in Medicare, Medicaid, or CHIP. |
2013–2016 |
· State & community-based models |
$984i |
|
State Innovation Models Initiative: Round Two – tested the effectiveness of financial, technical, and other support to states that were either prepared to test or were committed to designing and testing new payment and service delivery models for beneficiaries enrolled in Medicare, Medicaid, or CHIP. |
2015–2019 |
· State & community-based models |
$984i |
|
Strong Start for Mothers and Newborns Initiative: Enhanced Prenatal Care Models – tested three approaches to enhance care delivery and address the medical, behavioral, and psychosocial factors that may be present during pregnancy and contribute to preterm-related poor birth outcomes. |
2013–2017 |
· Health plan models |
$82 |
|
Treatment of Certain Complex Diagnostic Lab Tests Demonstration – tested the effect of making separate payments for certain complex diagnostic laboratory tests on access to care, quality of care, health outcomes, and expenditures. |
2012–2013 |
· Statutory demonstrations and other projects |
n/a |
|
Value in Opioid Use Disorder Treatment Demonstration – tested payments for care management and performance-based incentive payments for opioid use disorder treatment services aimed at increasing access to these services. |
2021–2024 |
· Statutory demonstrations and other projects |
n/a |
Legend: n/a = not applicable; tbd = to be determined
Source: CMS. | GAO‑26‑107953
aObligated amounts reflect commitments to participants in the testing of models, such as health care providers of services, states, conveners, and others. These commitments may include care management fees and cooperative agreement awards and were paid through Innovation Center funds as appropriated under section 1115A of the Social Security Act. Some statutory models were not funded through section 1115A obligations.
bAn ACO refers to a group of providers and suppliers of services, such as hospitals and physicians, that work together to coordinate care for the patients they serve. The Medicare Shared Savings Program is a voluntary program that encourages groups of doctors, hospitals, and other health care providers to form ACOs.
cAmount includes obligations for all four Bundled Payments for Care Improvement models.
dFederally qualified health centers provide comprehensive community-based primary and preventive care services in medically underserved areas or to medically underserved populations.
eAmount includes obligations for both the Global and Professional Direct Contracting Model and its successor ACO REACH Model.
fAmount includes obligations for both rounds one and two of the Health Care Innovation Awards models.
gAmount includes obligations for both the Home Health Value-Based Purchasing Model and its successor Expanded Home Health Value-Based Purchasing Model.
hAmount includes obligations for both phases of the Initiative to Reduce Avoidable Hospitalizations Among Nursing Facility Residents models.
iAmount includes obligations for both rounds one and two of the State Innovation Models Initiative.
GAO Contact
Leslie V. Gordon, GordonLV@gao.gov
Acknowledgments
In addition to the contact named above, Greg Giusto (Assistant Director), Kelly Krinn (Analyst-in-Charge), Leila Braun, Laura Elsberg, Ariel Landa-Seiersen, and Roxanna Sun made key contributions to this report.
The Government Accountability Office, the audit, evaluation, and investigative arm of Congress, exists to support Congress in meeting its constitutional responsibilities and to help improve the performance and accountability of the federal government for the American people. GAO examines the use of public funds; evaluates federal programs and policies; and provides analyses, recommendations, and other assistance to help Congress make informed oversight, policy, and funding decisions. GAO’s commitment to good government is reflected in its core values of accountability, integrity, and reliability.
Obtaining Copies of GAO Reports and Testimony
The fastest and easiest way to obtain copies of GAO documents at no cost is through our website. Each weekday afternoon, GAO posts on its website newly released reports, testimony, and correspondence. You can also subscribe to GAO’s email updates to receive notification of newly posted products.
Order by Phone
The price of each GAO publication reflects GAO’s actual cost of production and distribution and depends on the number of pages in the publication and whether the publication is printed in color or black and white. Pricing and ordering information is posted on GAO’s website, https://www.gao.gov/ordering.htm.
Place orders by calling (202) 512-6000, toll free (866) 801-7077,
or
TDD (202) 512-2537.
Orders may be paid for using American Express, Discover Card, MasterCard, Visa, check, or money order. Call for additional information.
Connect with GAO
Connect with GAO on X,
LinkedIn, Instagram, and YouTube.
Subscribe to our Email Updates. Listen to our Podcasts.
Visit GAO on the web at https://www.gao.gov.
To Report Fraud, Waste, and Abuse in Federal Programs
Contact FraudNet:
Website: https://www.gao.gov/about/what-gao-does/fraudnet
Automated answering system: (800) 424-5454
Media Relations
Sarah Kaczmarek, Managing Director, Media@gao.gov
Congressional Relations
David A. Powner, Acting Managing Director, CongRel@gao.gov
General Inquiries
[1]Congressional Budget Office, The Budget and Economic Outlook: 2025 to 2035, (Washington, D.C.: Jan. 2025). Medicare is the federal health insurance program for persons aged 65 or over, certain individuals with disabilities, and individuals with end-stage renal disease. Medicaid is a joint federal-state health care financing program for certain low-income individuals and medically needy individuals. CHIP is a federal-state program that provides health care coverage to children 18 years of age and younger living in low-income families whose incomes exceed the eligibility requirement for Medicaid.
[2]The Innovation Center was established by section 1115A of the Social Security Act, as added by section 3021 of PPACA. See Pub. L. No. 111-148, §§ 3021, 10306, 124 Stat. 119, 389, 939 (2010) (codified at 42 U.S.C. § 1315a).
[3]See appendix I for details on the delivery and payment approaches tested by the Innovation Center models.
[4]These appropriations remain available until expended.
[5]Congressional Budget Office, Federal Budgetary Effects of the Activities of the Center for Medicare & Medicaid Innovation, (Washington, D.C.: Sept. 2023).
[6]See GAO, CMS Innovation Center: Early Implementation Efforts Suggest Need for Additional Actions to Help Ensure Coordination with Other CMS Offices, GAO‑13‑12 (Washington, D.C.: Nov. 15, 2012). We also found that the Innovation Center had initiated implementation of a process to review and eliminate unnecessary duplication in the contracts awarded in one of its models. We recommended completing the implementation expeditiously. CMS implemented this recommendation in August 2013.
[7]GAO, CMS Innovation Center: Model Implementation and Center Performance, GAO‑18‑302 (Washington, D.C.: Mar. 26, 2018).
[8]The Innovation Center has implemented various initiatives that do not result in evaluations, which we did not count as models because these did not test a payment or delivery approach.
[9]Models tested and funded under section 1115A are those that are developed by the Innovation Center. Congress may also statutorily require CMS to test certain demonstrations, which may be operated by the Innovation Center. These statutorily required models may be funded separately from the section 1115A appropriations.
[10]For example, see Department of Health and Human Services, Center for Medicare and Medicaid Innovation, 2024 Report to Congress (Dec. 2024).
[11]GAO, Evidence-Based Policymaking: Practices to Help Manage and Assess the Results of Federal Efforts, GAO‑23‑105460 (Washington, D.C.: July 12, 2023), and Comparative Effectiveness Research: HHS Should Evaluate Its Performance of Related Activities, GAO‑25‑107462 (Washington, D.C.: July 14, 2025).
[12]See Medicare Payment Advisory Commission, Report to Congress: Aligning Incentives in Medicare (Washington, D.C.: 2010).
[13]44 U.S.C. §§ 3501-3520. The Office of Management and Budget assists the President in overseeing the preparation of the federal budget and in supervising its administration in executive branch agencies. It also oversees and coordinates the administration’s procurement, financial management, information, and regulatory policies.
[14]See GAO‑18‑302 for additional details on the Innovation Center’s process for model development and testing.
[15]Some models may be mandated by Congress.
[16]PTAC is an independent federal advisory committee chartered by HHS in 2016. Pub. L. No. 114-10, § 101(e)(1), 129 Stat. 115 (2015) (codified at 42 U.S.C. § 1395ee).
[17]Certain laws may also affect participation and model designs. For instance, rules related to the Stark law and anti-kickback statute—which restrict certain financial relationships among providers and referral practices in federally funded health care—were revised in 2021 to remove potential barriers to provider engagement in certain care coordination and value-based care arrangements. For example, the revised rules created a safe harbor under the anti-kickback statute for providers participating in Innovation Center value-based models, which previously required model-by-model waivers. Safe harbor regulations describe various payment and business practices that, although they could potentially implicate the anti-kickback statute, are not treated as offenses. However, Innovation Center officials could not quantify the effect of the updated rules on provider participation and told us these rules have helped the Innovation Center streamline its development of models. 85 Fed. Reg. 77,492 (Dec. 2, 2020); 85 Fed. Reg. 77,684 (Dec. 2, 2020).
[18]While the Office of the Actuary reviews the model evaluation, its analysis of expanded models may not result in the same findings because it differs in purpose and methods, according to Office of the Actuary officials.
[19]An obligation is a definite commitment that creates a legal liability of the government for the payment of goods and services ordered or received, or a legal duty on the part of the United States that could mature into a legal liability by virtue of actions on the part of the other party beyond the control of the United States. Payment may be made immediately or in the future.
[20]PPACA also appropriated $5 million to the Innovation Center in fiscal year 2010.
[21]The $10 billion appropriation from fiscal year 2020 was subject to sequestration, which reduced the amount provided in fiscal year 2020 by $590 million.
[22]Obligated amounts for individual models reflect commitments made to model participants (including health care providers, states, and others), if any, as well as other commitments to support model development and testing. Amounts do not include Medicare, Medicaid, and CHIP payments that health care providers or others receive for services provided to the beneficiaries.
[23]In addition, as we previously reported in GAO‑18‑302, officials noted that certain early models were expensive. For instance, the Health Care Innovation Awards and State Innovation Awards models provided funding to organizations and states, respectively, to test innovations.
[24]Participants are entities that have direct contractual relationship with CMS to implement the model, and providers are typically Medicare-enrolled providers and suppliers, such as individual clinicians, that engage in models through the participant, according to CMS officials.
[25]Arrangements between CMS, states, and other participants vary by model. For example, in the Cell and Gene Therapy Access Model, CMS partners with participating state Medicaid programs and with drug manufacturers. In the Innovation in Behavioral Health Model, CMS partners with participating state Medicaid programs that in turn recruit providers to participate.
[26]Other models that included payers in addition to health care provider organizations or states are included in tables 2 and 3 in this report.
[27]Models may achieve savings during testing according to evaluations but not be expanded. Three other models (Accountable Care Organization Investment Model, Maryland All-Payer Model, and Medicare Care Choices Model) achieved net savings in testing. These models were not expanded for various reasons including limited participation, according to officials.
[28]42 U.S.C. § 1315a(b)(4)(A)(i).
[29]The nine successor models include two expanded models within the Innovation Center portfolio. In March 2025, the Innovation Center announced that, following a data-driven review of the model portfolio, it planned to end four of the nine successor models by the end of 2025.
[30]The Increasing Organ Transplant Access Model began testing on July 1, 2025. The Transforming Episode Accountability Model began testing on January 1, 2026.
[31]The Kidney Care Choices and End-Stage Renal Disease Treatment Choices models were themselves successor models that built upon the earlier Comprehensive End-Stage Renal Disease Care Model.
[32]The Medicare Shared Savings Program is a voluntary program that encourages groups of doctors, hospitals, and other health care providers to form ACOs.
