Report to Congressional Committees
United States Government Accountability Office
A report to congressional committees
For more information, contact: Alyssa M. Hundrup at hundrupa@gao.gov
What GAO Found
The Veterans Health Administration’s (VHA) Caregiver Support Program offers mental health support, among other benefits, to eligible caregivers who provide around the clock care for veterans with serious injuries. This includes support groups and respite care. In fiscal year 2025, VHA data show the program served about 98,000 caregivers. In addition, VHA obligated $2.6 billion to implement the program, according to officials. VHA officials told GAO the program has grown significantly since fiscal year 2021 due in part to expanded eligibility criteria that allowed more caregivers to participate as of October 1, 2020.
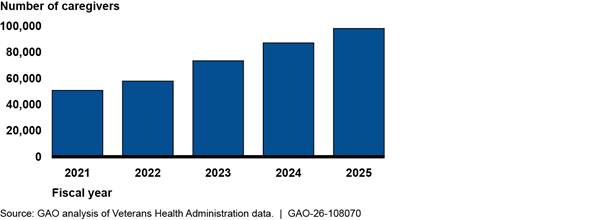
Caregivers Participating in Veterans Health Administration Caregiver Support Program, Fiscal Years 2021 Through 2025
VHA advertises the Caregiver Support Program through various methods, such as email updates and brochures at Department of Veterans Affairs (VA) medical centers. Some caregivers GAO interviewed said they learned about the program through these methods. However, they wished they had learned about it sooner. They also felt other caregivers did not know about the mental health support available to them through the program.
VHA established four goals to assess whether its outreach efforts are effective at increasing caregivers’ awareness of the program. One goal is to increase program enrollment by 15 percent each fiscal year. However, the other three goals, such as increasing subscribers to its email updates, do not have quantitative targets and time frames. Setting targets and time frames for these goals would better enable VHA to measure its progress in increasing awareness of the program among caregivers who are not enrolled, help the agency assess how well its outreach efforts are working, and make any needed adjustments.
VHA has also taken steps to assess how the program supports caregivers by establishing a goal to increase telehealth appointments by 10 percent in fiscal year 2025. VHA collects data on these appointments, which increased by 50 percent from fiscal year 2024 to 2025. However, the agency has not established goals and collected related data for other program services, such as other types of mental health treatment. Setting goals and collecting more complete information would better position VA to assess program performance. VHA could make any needed adjustments to further support caregivers’ wellbeing, allowing it to better support veterans.
Why GAO Did This Study
Several factors, including the demands of their care duties, can affect caregivers’ mental health and wellbeing. Research suggests that such caregiving can be linked to high levels of stress and burden and can result in depression or anxiety.
The Senator Elizabeth Dole 21st Century Veterans Healthcare and Benefits Improvements Act includes a provision for GAO to review mental health support provided by the VHA Caregiver Support Program. This report examines VHA’s efforts to make caregivers aware of the mental health support available to them and VHA’s efforts to assess program performance, among other objectives.
GAO reviewed VHA documentation and data for fiscal years 2021 through 2025. GAO also interviewed VHA officials, program staff and selected caregivers at four VA medical centers, and representatives from four organizations serving veterans and caregivers. GAO selected the medical centers based on program size, geography, and rurality. GAO selected organizations that focus on caregivers and have national reach. GAO also conducted a literature search and review of relevant research.
What GAO Recommends
GAO is making two recommendations to VA to implement key performance management practices for the Caregiver Support Program, including setting quantitative targets and time frames for outreach goals, and setting goals and collecting relevant data to assess services the program offers to support caregivers’ mental health. VA concurred with the recommendations and identified steps VHA plans to take to implement them.
|
Abbreviations |
|
|
|
VA |
Department of Veterans Affairs |
|
|
VHA |
Veterans Health Administration |
|
This is a work of the U.S. government and is not subject to copyright protection in the United States. The published product may be reproduced and distributed in its entirety without further permission from GAO. However, because this work may contain copyrighted images or other material, permission from the copyright holder may be necessary if you wish to reproduce this material separately.
April 16, 2026
The Honorable Jerry Moran
Chairman
The Honorable Richard Blumenthal
Ranking Member
Committee on Veterans’ Affairs
United States Senate
The Honorable Mike Bost
Chairman
The Honorable Mark Takano
Ranking Member
Committee on Veterans’ Affairs
House of Representatives
Many U.S. veterans have suffered serious injuries in the line of duty and often rely on assistance from caregivers, including family members. Such caregivers typically assist veterans with tasks of everyday living, like bathing and eating, as well as help with making medical, legal, or financial decisions. This assistance can help veterans to achieve a better quality of life and contribute to their recovery. However, researchers and others have identified concerns about the mental health and wellbeing of caregivers of veterans.[1] Caregivers often provide care continuously, which can lead to high levels of stress and burden, and limit their ability to care for themselves. As a result, such caregiving can take a toll on caregivers’ mental health and may result in conditions like depression and anxiety. For example, one study found that 43 percent of caregivers of servicemembers or veterans aged 60 or younger met criteria for depression.[2]
To support caregivers of veterans, the Veterans Health Administration (VHA) established the Caregiver Support Program in 2011. Through this program, VHA offers self-care education and resources to support eligible caregivers’ mental health and wellbeing, such as support groups and respite care, among other benefits. In fiscal year 2025, VHA obligated about $2.6 billion to implement the Caregiver Support Program, according to VHA officials, and served nearly 100,000 caregivers.
The Senator Elizabeth Dole 21st Century Veterans Healthcare and Benefits Improvement Act includes a provision for us to review VHA’s efforts to provide mental health support for caregivers of veterans.[3] In this report, we
1. describe the factors that can affect caregivers’ mental health and wellbeing;
2. describe the mental health support VHA offers caregivers, and actions it has taken to address challenges caregivers may face obtaining support;
3. examine VHA’s efforts to make caregivers aware of the Caregiver Support Program and available mental health support; and
4. examine VHA’s efforts to assess how the Caregiver Support Program is supporting caregivers’ mental health.
To answer the first objective, we conducted a literature search and reviewed relevant research published between 2020 and 2025 to identify factors that can affect caregivers’ mental health and wellbeing.[4] To answer the other three objectives, we obtained data from VHA on the Caregiver Support Program for fiscal years 2021 through 2025 (the most recent data at the time of our review). These included data on the number and characteristics of caregivers participating in the program, and those caregivers who had received mental health treatment. To assess the reliability of these data, we interviewed relevant agency officials and reviewed the data for obvious errors. On the basis of these steps, we determined the data were sufficiently reliable for the purposes of our reporting objectives. Additional information on our analysis of VHA data and literature review is in appendix I. For a complete list of literature we reviewed, see the bibliography at the end of this report. In addition, we reviewed VHA documentation on the Caregiver Support Program and mental health support it offers.
To answer all four objectives, we interviewed VHA officials from the national Caregiver Support Program Office who are responsible for overseeing the program and providing guidance to Department of Veterans Affairs (VA) medical centers implementing the program. We also interviewed Caregiver Support Program staff who operate the program at a nongeneralizable selection of four VA medical centers.[5] We selected these VA medical centers to obtain variation in geography, rurality, and the number of caregivers participating in the Caregiver Support Program.
Across the four medical centers, we also conducted eight discussion groups with a selection of 50 caregivers participating in the Caregiver Support Program to understand caregiver experiences obtaining mental health support from the program. We worked with VA medical center staff to identify and conduct outreach to caregivers to participate in these discussion groups. Lastly, we interviewed officials from two veterans service organizations and two foundations that serve veterans and their caregivers.[6] We selected these organizations and foundations based on their focus on caregivers of veterans, knowledge of the Caregiver Support Program, and national reach. Information we obtained from these discussion groups and interviews is not generalizable across caregivers or VA medical centers but rather provides illustrative examples of a variety of experiences from caregivers and staff. Additional information about the documentation we reviewed and interviews we conducted is in appendix I.
To examine VHA’s efforts to make caregivers aware of the Caregiver Support Program and available mental health support, we evaluated VHA’s efforts to assess how it disseminates information on the program against performance management criteria to determine the extent to which these efforts are consistent with key performance management practices we identified in prior work.[7] Specifically, these criteria define performance management as a three-step process by which agencies (1) set goals with quantitative targets and time frames to identify the results they seek to achieve, (2) collect performance information to measure progress towards meeting its goals, and (3) use that information to assess results and inform decisions to ensure further progress towards achieving its goals.
In addition, to examine VHA’s efforts to assess how the program is supporting caregivers’ mental health, we evaluated its efforts against these same performance management criteria to determine the extent to which these efforts are consistent with key performance management practices.[8] Additional information about our assessment of VHA’s efforts is in appendix I.
We conducted this performance audit from January 2025 to April 2026 in accordance with generally accepted government auditing standards. Those standards require that we plan and perform the audit to obtain sufficient, appropriate evidence to provide a reasonable basis for our findings and conclusions based on our audit objectives. We believe that the evidence obtained provides a reasonable basis for our findings and conclusions based on our audit objectives.
Background
Caregiver Support Program Administration and Components
The Caregivers and Veterans Omnibus Health Services Act of 2010 requires VA to establish a program to assist caregivers with caring for veterans.[9] VHA established the Caregiver Support Program in May 2011. The program’s mission is to promote the health and well-being of family caregivers who care for veterans, through education, resources, support, and services, according to VHA’s website.
Within VHA, the Caregiver Support Program Office administers the program at the national level and individual VA medical centers administer the program locally.
· The national Caregiver Support Program Office is responsible for developing policies, procedures, and program offerings that VA medical centers use to support caregivers, such as self-care courses and educational materials. In addition, the Caregiver Support Program Office, in conjunction with regional offices, provides guidance, oversight, and support to VA medical centers, such as recommending best practices for implementing the program.
· Caregiver Support Program staff at the 173 VA medical centers across the VHA health care system are responsible for identifying and coordinating support to caregivers enrolled in their specific catchment area, recommending relevant VA or community programs to caregivers, and overseeing the enrollment process. These staff generally include clinical staff such as social workers, nurses, and psychologists, as well as administrative staff. Additionally, VA medical centers may choose to develop and offer services in addition to those provided by the national office.
The Caregiver Support Program consists of two components—the Program of General Caregiver Support Services (general component) and the Program of Comprehensive Assistance for Family Caregivers (comprehensive component).[10] These components vary in their eligibility criteria and services offered. Caregivers of any veteran enrolled in the VHA health care system can join the general component. In contrast, the comprehensive component requires that for the caregiver to participate, the veteran and caregiver must meet certain criteria (see table 1).
|
|
Program of General Caregiver Support Services (general component) |
Program of Comprehensive Assistance for Family Caregivers (comprehensive component) |
|
Fiscal year 2025 enrollment |
Approximately 28,800 caregivers |
Approximately 70,000 caregivers |
|
Eligibility |
Caregiver of veteran from any era enrolled in VHA health care |
· Caregiver of veteran from any era with at least a 70 percent service-connected disability rating and in need of in-person personal care services for a minimum of 6 continuous monthsa,b · Caregiver is at least 18 years old · Caregiver is a relative of or lives full-time with the veteran · Caregiver passes an assessment and completes caregiver education and training |
|
Services |
Offers general support such as peer support mentoring, respite care, skills training, coaching, telephone support through the Caregiver Support Line, online programs, and exploring available mental health resources in the community, such as help finding mental health counseling. |
Offers the same support as the Program of General Caregiver Support Services, plus: · Monthly stipend and travel benefits · Civilian Health and Medical Program of the Department of Veterans Affairs health benefits coverage, if otherwise uninsured · Mental health treatment · Legal and financial planning services |
Source: GAO analysis of Veterans Health Administration documentation and data. | GAO‑26‑108070
aCaregivers of veterans who served after September 11, 2001, have been eligible for the comprehensive component since it was established in 2011. Veterans who served before May 7, 1975, became eligible as of October 1, 2020, and veterans who served between May 7, 1975, and September 11, 2001, became eligible as of October 1, 2022.
bFor purposes of the Caregiver Support Program, the Department of Veterans Affairs considers a veteran to have this level of need if the veteran is unable to perform an activity of daily living, needs supervision or protection based on symptoms or residuals of neurological or other impairment or injury, or needs regular or extensive instruction or supervision without which the ability of the veteran to function in daily life would be seriously impaired, according to Caregiver Support Program guidance.
The process to enroll in the Caregiver Support Program varies for the two program components, according to Caregiver Support Program Office guidance. For example, to enroll in the general component, caregivers contact their local VA medical center and complete an intake with program staff. To participate in the comprehensive component, caregivers must submit an application, complete an assessment of their ability to provide personal care services to the veteran, and receive approval based on eligibility criteria.[11] Caregiver Support Program Office guidance states that VA medical center staff should offer caregivers to enroll in the general component while waiting for their eligibility to be determined for the comprehensive component, or if their application is denied.
Once caregivers are approved to participate in the comprehensive component, VHA regulations require Caregiver Support Program staff at VA medical centers to periodically conduct wellness contacts to monitor the caregiver’s health and wellbeing, among other things. Staff are to conduct wellness contacts every 120 days for caregivers participating in the comprehensive component, with at least one wellness contact occurring in the veteran’s home once a year.[12] Staff may also conduct wellness contacts virtually.
Caregiver Support Program staff contact caregivers enrolled in the general component annually to assess their needs and provide support based on their needs. Additionally, VA medical center staff reassess caregivers’ continued eligibility for the comprehensive component at the request of the veteran or caregiver.[13]
Participation in the Caregiver Support Program
VHA data show that in fiscal year 2025, about 98,000 caregivers participated in the Caregiver Support Program, nearly double the number of caregivers who participated in fiscal year 2021 (see fig. 1).
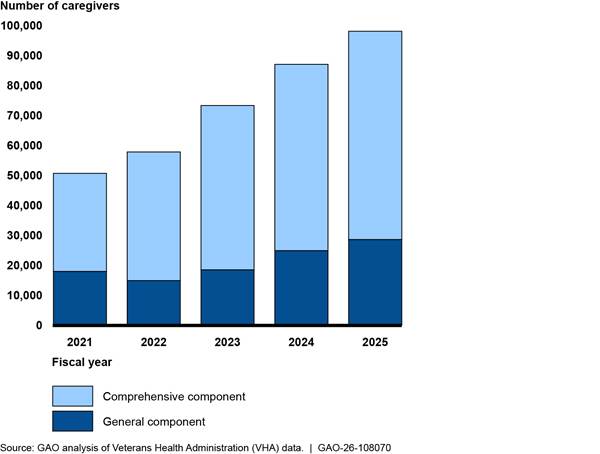
Notes: The Caregiver Support Program consists of two separate components to support caregivers of veterans: the Program of General Caregiver Support Services (general component) and the Program of Comprehensive Assistance for Family Caregivers (comprehensive component). Caregivers of any eligible veteran enrolled in VHA health care may enroll in the general component. Caregivers must apply for the comprehensive component and meet certain criteria (e.g., the veteran must meet a certain level of need) to participate. VHA established the Caregiver Support Program in 2011. However, eligibility for the comprehensive component expanded to allow more caregivers of veterans to participate in the program beginning October 1, 2020. As a result, VHA data on enrollment prior to fiscal year 2021 is not comparable to data for fiscal years 2021 through 2025, according to VHA officials.
According to Caregiver Support Program Office officials, the increase in participation resulted from expanding eligibility for the comprehensive component as of fiscal year 2021, under the VA MISSION Act of 2018.[14] Officials from the Caregiver Support Program Office said VA has requested annual program funding based on estimated projections of growth, including anticipating increases in enrollment after more caregivers of veterans became eligible for the comprehensive component.[15] For example, VA received $874.5 million in funding for the Caregiver Support Program for fiscal year 2021 (the first full year of expanded eligibility), approximately double the $437.9 million it received in fiscal year 2019 (the last full year before eligibility expanded), according to VA officials. In its fiscal year 2026 budget submission, VA requested $3.3 billion for the program for fiscal year 2026 and $3.6 billion for fiscal year 2027 to support further anticipated increases in enrollment.[16] The majority of program spending is for stipends and benefits VA pays to caregivers in the comprehensive component for their caregiving duties.[17]
According to VHA data, the majority of caregivers participating in the Caregiver Support Program in fiscal year 2025 were female and a spouse or partner of the veteran. In addition, in fiscal year 2025, most caregivers were between ages 50 and 80. See figure 2 for more information on caregivers’ sex, age, and relationship to the veteran. Further, some caregivers are also veterans. According to Caregiver Support Program officials, as of January 2026, approximately 7,300 of the 98,000 (just over 7 percent) caregivers participating in the program were also veterans.
Figure 2: Percentage of Caregivers Participating in VHA Caregiver Support Program by Program Component and Sex, Age, and Relationship to Veteran, Fiscal Year 2025
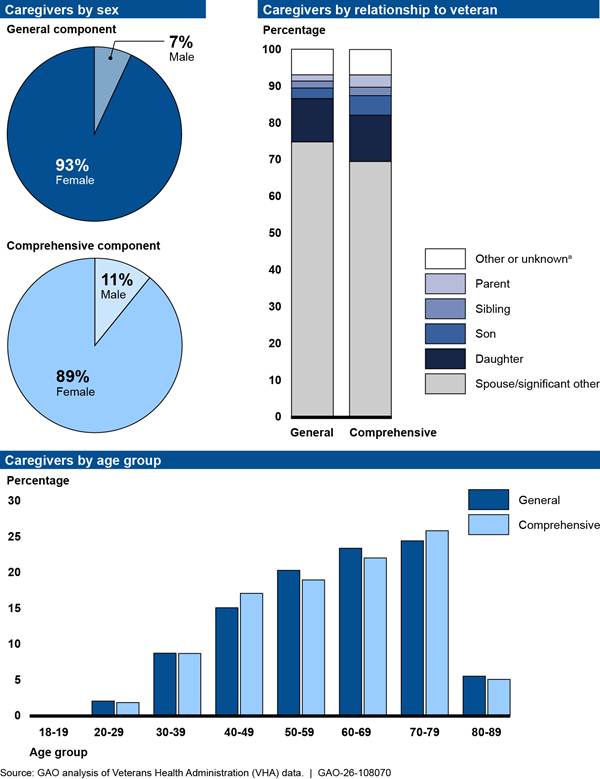
Notes: The Caregiver Support Program consists of two components: the Program of General Caregiver Support Services (general component) and the Program of Comprehensive Assistance for Family Caregivers (comprehensive component). Caregivers of any eligible veteran enrolled in VHA health care may enroll in the general component. Caregivers must apply for the comprehensive component and meet certain criteria (e.g., the veteran must meet a certain level of need) to participate. Less than 1 percent of caregivers in either program were age 90 and older in fiscal year 2025.
aOther relationships that caregivers of veterans may have include grandchildren, other relatives, and friends. In fiscal year 2025, relationship to the veteran was unknown for about 2 percent of caregivers in the general component and 0 percent of caregivers in the comprehensive component.
Various Factors Such as Stress, Burnout, and Isolation Can Affect Caregivers’ Mental Health and Wellbeing
Based on our literature review and interviews with Caregiver Support Program officials, VA medical center staff, and caregivers at four selected VA medical centers, we identified several factors that can negatively affect caregivers’ mental health and wellbeing, as shown in table 2. The literature and caregivers we interviewed most commonly cited stress and burnout, in part based on the continuous and extensive nature of care that is often required of caregivers. In addition, caregivers noted feeling isolation.
Table 2: Examples of Factors That Can Affect the Mental Health and Wellbeing of Caregivers of Veterans
|
Factors affecting the mental health of caregivers of veterans |
Examples from literature review |
Examples from caregiver interviews |
|
Stress and burnout |
· Suppressing emotions or “hypervigilance” (means of managing emotion) may contribute to emotional distress and decreased well-being among caregivers. · A larger share of caregivers of younger veterans reported experiencing stress. For example, 75 percent of veteran caregivers caring for someone 60 or under reported experiencing stress, compared to 44 percent among those caring for a veteran 60 or over. |
· Caregivers noted feeling stressed, frustrated, or burned out. · Caregivers said they often cannot get a day off from caregiving or cannot leave their veteran alone. · Caregivers noted that their veterans do not want another person to care for them, which makes the caregivers feel like they cannot leave their veterans. |
|
Financial insecurity |
· Caregivers exhibiting high amounts of distress (roughly one in five) reported the lowest levels of well-being and financial security. · Caregivers said they struggled to pay their bills each month, with 40 percent reporting that they had trouble affording food. |
· Caregivers said they stopped working to become full-time caregivers. · Caregivers noted the veteran they care for had to stop working because of their condition. |
|
Not caring for self |
· As many as one in three caregivers had not sought the mental health care they needed, indicating they did not have time. Further, caregivers providing care to those 60 and under are at greater risk of depression and are less likely to seek care. · Caregivers who are veterans themselves and who participate in the comprehensive caregiver program are more likely to seek health care. |
· Caregivers noted that they struggled to focus on their own health and needs because of their caregiving duties. For example, one caregiver was hospitalized due to stress. Another said she did not feel worthy of seeking support for herself because her husband went to war and risked his life, so she focused on caring for him. |
|
Loss of self or planned life |
· Caregivers exhibiting high or moderate amounts of distress reported higher loss of self and odds of suicide ideation. · In addition, caregivers reported experiencing disruption in their lives and relationships compared to caregivers of non-veterans. |
· Caregivers said they felt they lost who they were because of their caregiving. For example, some said others in their lives do not ask how they are doing. · Caregivers said they felt sadness and grief, noting that they were “pushed into” caregiving and that the role does not happen by choice. Other caregivers said they experience grief over the veteran’s condition and losing how they thought the rest of their life would be. |
|
Isolation |
· Caregivers reported experiencing feelings of loneliness, especially among those who experienced higher levels of burden. · Following medical emergencies, caregivers reported they no longer participated in activities outside the home and withdrew from social activities. |
· Caregivers reported experiencing isolation, with caregivers at one medical center saying isolation was their primary mental health issue. Caregivers said that they cannot go out and do what they would like to, such as traveling to visit family. · Some caregivers said that they feel isolated because they are unable to travel and see friends or family who do not live nearby. |
|
Difficulty sleeping |
· About half of caregivers reported having difficulty sleeping, averaging less than 7 hours of sleep a night. |
· Caregivers said they had difficulty sleeping at night, waking up multiple times throughout the night, and noting that they felt they needed to be alert in case their veterans had an emergency. |
|
Family and needs for children |
· Caregivers of veterans reported experiencing more family disruption than caregivers of civilians. · Caregivers reported needing more support for their children, who often share caregiving duties and have unmet mental health needs themselves. · Having multiple caregiving roles such as school-aged children or aging parents, is associated with greater stress and strain. |
· Some caregivers discussed that having children in the household affects their caregiving duties and children’s mental health. For example, one caregiver noted that it is difficult for her children to go to school while dealing with the veteran’s mental health issues, and children do not have friends visit, which can be isolating. · One caregiver said her children feel sad when the veteran’s condition worsens. · Some caregivers caring for parents said it can be difficult to balance caregiving with other responsibilities. For example, one caregiver said she was not able to help plan her daughter’s wedding due to her responsibilities as a caregiver. |
Source: GAO analysis of literature and interviews with caregivers. | GAO‑26‑108070
Note: We conducted a structured search of peer-reviewed articles and research organization reports using various terms related to our objective, such as “caregiver,” “veteran,” and “mental health.” We reviewed the facts presented, population studied, and methodology used, including any limitations, and identified 16 articles that were relevant and methodology sound. We analyzed these 16 articles to identify themes. We also conducted interviews with a non-generalizable sample of 50 caregivers of veterans as part of eight discussion groups at four Department of Veterans Affairs medical centers, which we selected for variation in geography, size of Caregiver Support Program, and rurality. Information presented here reflects examples from the broader themes we heard across our discussion groups and may not reflect caregiver perspectives of all those included in the discussion groups or other caregivers generally.
Officials from a veterans service organization, a foundation, and VA medical centers echoed the factors cited in the literature and by caregivers we interviewed. For example, Caregiver Support Program staff at three of the four VA medical centers in our review said caregivers might experience burnout or stress, isolation, or grief, such as mourning the loss of their relationship with the veteran or the life they thought they would have. In addition, officials from one veterans service organization and one foundation highlighted factors such as financial instability and stress on family. Officials from one veterans service organization we interviewed stated that although some caregivers were eligible for monthly stipends, these payments were often insufficient to cover costs, such as their veterans’ medical expenses, which caused additional stress. An official from one foundation noted the significant effort caregivers invest trying to receive support and recognition as a caregiver can strain their relationships with the veteran they are caring for.
VA medical center staff said these factors can contribute to mental health conditions. Officials from the Caregiver Support Program Office said they see a wide range of mental health needs among caregivers, but most commonly see depression and anxiety. For example, officials said the work caregivers do could also lead to anxiety in that caregivers are caring for a sick or disabled loved one and working to ensure their veterans’ needs are met. Caregivers of veterans who we spoke with at three VA medical centers also noted feeling anxious or depressed. For example, caregivers described feeling anxious in anticipation of the loss of their veteran or in seeing their condition worsen.
VHA Offers Caregivers Various Services to Improve Mental Health and Has Responded to Challenges Raised by Caregivers
VHA Caregiver Support Program Offers Services to Improve Mental Health and Wellbeing, Such as Self-Care Education and Respite Care
VHA offers various types of support to caregivers of veterans through the Caregiver Support Program to enhance their mental health and wellbeing, according to VHA documentation and officials (see table 3). Caregivers participating in the comprehensive component may be eligible to receive mental health treatment, while all other services listed in table 3 are available to caregivers in both the general and comprehensive components.
|
Type of support |
General |
Comprehensive component |
|
Supportive messages from the Annie Caregiver Text Program: Caregivers can sign up to receive educational and supportive messages from Annie, the Department of Veterans’ Affairs (VA) text messaging service, to help manage stress and take care of themselves. |
☑ |
☑ |
|
Emotional support and referrals to Caregiver Support Program staff from Caregiver Support Line: The Caregiver Support Line is a toll-free number that caregivers may contact to obtain information on available services, referrals to support, and emotional support. The line operates from 8 a.m. to 8 p.m. Eastern Time. |
☑ |
☑ |
|
Self-care coaching: Caregivers can participate in coaching programs through the Caregiver Support Program to help with issues caregivers face and enhance their physical, emotional, and mental health. |
☑ |
☑ |
|
Self-care education and workshops: The caregiver support program offers resources that provide caregivers with education on caring for themselves, in addition to caring for their veteran. These resources are available in-person and virtually, and include courses on self-care, resilience, and suicide prevention; workshops to help manage emotions like stress and anxiety, as well as substance use or sleep challenges; and relaxation and self-care techniques like yoga, art journaling, or listening to music. |
☑ |
☑ |
|
Emotional support and recommendations to other services from Caregiver Support Program staff: Caregiver Support Program staff provide emotional support, active listening, encouragement, guidance, coping strategies, and education to caregivers individually and through support groups. Staff can also refer caregivers to other services. |
☑ |
☑ |
|
Mental health treatment: Caregivers can receive individual, group, couples, or family therapy, at a VA medical center or through the Virtual Psychotherapy Program for Caregivers, to address stress and other psychological concerns. The Virtual Psychotherapy Program for Caregivers was established in fiscal year 2023 in collaboration with Veterans Integrated Service Networks, according to Caregiver Support Program officials. Caregivers do not receive medication through this service. The program was operational in all regions by June 2024, according to Caregiver Support Program officials. |
—a |
☑ |
|
Respite care to provide breaks from caregiving: Respite care provides short-term and intermittent relief to caregivers, which allows them to take a break from their caregiving responsibilities. Caregivers are eligible for no less than 30 days of respite care per year. Respite for caregivers in the general component is offered through VA’s Office of Geriatrics and Extended Care, which determines the clinically appropriate amount of care. Respite for caregivers in the comprehensive component is offered through the Caregiver Support Program, in consultation with the veterans’ providers, and includes more than 30 days of respite per year. |
☑ |
☑ |
Source: GAO analysis of Veterans Health Administration (VHA) information. | GAO‑26‑108070
Notes: The Caregiver Support Program consists of two separate components: the Program of General Caregiver Support Services (general component) and the Program of Comprehensive Assistance for Family Caregivers (comprehensive component). Caregivers of any eligible veteran enrolled in VA health care may enroll in the general component. Caregivers must apply for the comprehensive component and meet certain criteria (e.g., the veteran must meet a certain level of need) to participate.
aThe Caregiver Support Program does not offer mental health treatment to caregivers participating in the general component of the caregiver program, unless it is necessary to support the veteran’s treatment, such as couples’ counseling, or if they are a veteran eligible for and receiving health care through VHA.
Caregiver Support Program Office officials said they use surveys, listening sessions, and wellness contacts to identify caregivers needs, and use that information to determine which services to offer through the program. Similarly, Caregiver Support Program staff we interviewed at selected VA medical centers said they may decide to offer certain types of support based on the local needs of the caregivers they serve, such as support groups for caregivers of veterans with certain diagnoses.
According to program officials and staff at one selected VA medical center, caregivers can choose which program services they would like to use, depending on their needs and preferences. For example, caregivers we interviewed at selected VA medical centers found support groups to be helpful and participated in various groups where they connected with other caregivers and offered each other support, such as coffee meetups and a gardening group. In addition, caregivers can choose to receive services in person or virtually for some of the options, such as support groups that some medical centers offer over video call or in person. Caregivers we interviewed at selected VA medical centers said they use both options.
|
VHA Data on Caregivers’ Mental Health VHA data on caregivers participating in the comprehensive component give some insight into their mental health needs. For instance, in fiscal years 2022 through 2025, anxiety and depression-related disorders were the two most common diagnoses, according to VHA data. In fiscal year 2025 specifically, 32 percent of caregivers in the comprehensive component who received mental health treatment through VHA had a diagnosis for an anxiety-related disorder, and 26 percent of these caregivers had a depression-related disorder diagnosis. The third-most common diagnosis among caregivers in the comprehensive component who received mental health treatment through VHA in fiscal years 2022 through 2025 was post-traumatic stress disorder. Source: GAO analysis of Veterans Health Administration (VHA) data. | GAO‑26‑108070 |
Mental health treatment, such as individual psychotherapy, is one of the main services VHA provides caregivers participating in the comprehensive component, according to officials from the Caregiver Support Program Office.[18] These caregivers may receive mental health treatment through their VA medical centers or the Virtual Psychotherapy Program for Caregivers. This program provides telehealth therapy for caregivers participating in the comprehensive component, including individual, group, and couples or family therapy. From fiscal year 2021 through 2025, the number of caregivers in the comprehensive component who had an encounter within VHA for mental health treatment tripled, according to VHA data (see fig. 3). The percentage of caregivers in the comprehensive component who had such an encounter also increased during this time, from 6 percent of caregivers in fiscal year 2021 to 9 percent in fiscal year 2025. Officials stated the increase in the number and percentage of caregivers with a mental health encounter is due to the implementation of the Virtual Psychotherapy Program for Caregivers in fiscal year 2023, in addition to program growth.
Figure 3: Number of Caregivers in the Comprehensive Component of the Caregiver Support Program with a Mental Health Encounter within the Veterans Health Administration, Fiscal Year 2021 – 2025
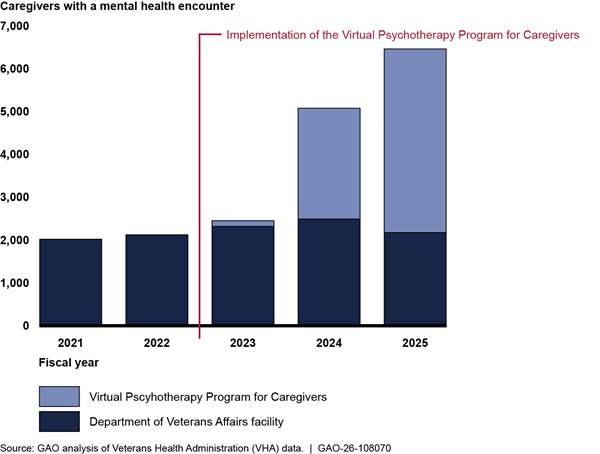
Note: Caregivers must apply for the comprehensive component and meet certain criteria (e.g., the veteran must meet a certain level of need) to participate and receive mental health treatment. Caregiver Support Program officials said they implemented the Virtual Psychotherapy Program for Caregivers in phases starting in fiscal year 2023 through fiscal year 2024.
In addition, Caregiver Support Program staff at VA medical centers can provide caregivers with recommendations to other mental health support not offered through the program. For example, they could help caregivers identify programs or mental health providers in the community. Officials from the Caregiver Support Program Office said they are unable to track mental health support that caregivers receive in the community, unless the caregiver is also a veteran who receives care through the Veterans Community Care Program.[19] VHA data do not capture information on care from non-VHA providers beyond community care claims, according to these officials, because VHA does not pay for this care.
Caregivers Identified Several Challenges Obtaining Mental Health Support; VHA Steps to Address These Include Establishing a Virtual Therapy Program
Caregivers we interviewed at the four selected VA medical centers said they appreciated the mental health support that the Caregiver Support Program offers. However, caregivers also noted experiencing some challenges obtaining this support, such as being unable to travel to the VA medical center for in-person services (see table 4).
Table 4: Examples of Challenges Caregivers of Veterans Experience Obtaining Mental Health Support in Caregiver Support Program
|
Unable to travel to the Department of Veterans Affairs (VA) medical center. Some caregivers identified going to VA medical centers as a challenge to accessing mental health support in person. Specifically, caregivers may not have transportation or live near a VA medical center, resulting in a long drive. Caregivers also said they may not be able to leave their veteran alone while they are gone. |
|
Limited staffing for desired services. Caregivers wished they had more opportunities to participate in program services, such as more frequent support group meetings, but expressed concerns that VA medical centers did not have enough staff to provide additional group meetings. Some caregivers also thought that more options for individual therapy would be helpful to all caregivers. |
|
Difficulty accessing high quality respite care. Caregivers reported challenges accessing respite care, including limited availability for in-home respite care, concerns about the quality of respite care, or limited awareness of the Caregiver Support Program’s respite care offerings. |
|
Limited digital literacy. Caregivers reported challenges using technology, such as VA’s videoconferencing software, to attend virtual events. |
Source: GAO analysis of interviews with caregivers. | GAO‑26‑108070
Note: We conducted interviews with 50 caregivers of veterans from eight discussion groups at four VA medical centers, which we selected based on geography, size of Caregiver Support Program, and rurality. Information presented here reflects examples from the broader themes we heard across our discussion groups, and may not reflect caregiver perspectives of all those included in the discussion groups or other caregivers generally.
Caregiver Support Program Office officials and some VA medical center staff we spoke with told us they have taken some steps to address the challenges caregivers reported, including the following:
· Offering some virtual services, such as virtual support groups, in response to caregivers’ limited ability to travel and preferences for services they could participate in from home, according to Caregiver Support Program Office officials.
· Creating the Virtual Psychotherapy Program for Caregivers in fiscal year 2023, according to Caregiver Support Program Office officials. This program provides caregivers in the comprehensive component the option to receive mental health treatment virtually. Caregiver Support Program Office officials said that previously, caregivers seen for therapy primarily received individual therapy in person at a VA medical center. The Virtual Psychotherapy Program for Caregivers aims to address capacity challenges among mental health providers at VA medical centers, according to Caregiver Support Program Office officials and staff at two VA medical centers. In addition, officials said the Virtual Psychotherapy Program for Caregivers also helps address challenges caregivers face traveling to VA medical centers because it exclusively offers virtual appointments.
· Monthly monitoring and documentation of caregivers’ use of respite care at each VA medical center. According to this requirement, which regional Caregiver Support Program staff monitor, VA medical centers with low respite care utilization must have a plan to ensure caregivers are educated about the availability of respite care.
· Offering in-person services at VA medical centers and providing on-site staff support during business hours for caregivers who prefer to receive support in-person. In addition, program staff at one VA medical center said they connect caregivers with VA resources to troubleshoot technology issues and help them become more comfortable with videoconferencing.
Additionally, the Caregiver Support Program Office has considered expanding access to mental health treatment—equivalent to the comprehensive component—to address challenges those in the general component have reported in receiving such care. As described above, only caregivers participating in the comprehensive component can receive individual, group, or couples or family therapy in person at a VA medical center or through the Virtual Psychotherapy Program for Caregivers. Officials from the Caregiver Support Program Office said they understood that they do not have the legal authority to offer this service for the general component, as they do for the comprehensive component.
However, VA medical center staff we interviewed said there is a need for mental health treatment for all caregivers. Caregiver Support Program staff at three selected VA medical centers noted the importance of mental health treatment and expressed disappointment that caregivers in the general component cannot access it. Caregivers we interviewed agreed that it would be beneficial for caregivers in the general component to have access to mental health treatment through the Caregiver Support Program. Furthermore, caregivers we spoke with enrolled in the general component reported feeling burned out and depressed.
In September 2025, the Caregiver Support Program Office assessed expanding eligibility for mental health treatment to the general component. Its assessment estimated that up to 1,622 additional caregivers would choose to receive mental health treatment as a result of an expansion.[20] As of January 2026, VA officials stated they are reviewing the program office’s assessment to evaluate whether legislative authority is needed to expand eligibility for mental health treatment to the general component.
VHA Advertises Support for Caregivers, But Has Not Fully Assessed Effectiveness of Its Efforts
VHA Uses Several Methods to Spread Awareness of Caregiver Support Program and Its Mental Health Support Offerings
The Caregiver Support Program Office spreads awareness of the program and the mental health support it offers to caregivers of veterans using various methods. The program uses each method with varying frequency, from annual resource fairs to monthly newsletters, according to Caregiver Support Program Office documentation and officials. See table 5 for a list of the methods VHA uses to advertise the Caregiver Support Program and the frequency of each method.
Table 5: Veterans Health Administration (VHA) Methods to Advertise Caregiver Support Program and Frequency of Each Method
|
VHA’s Method |
Frequency of Method |
|
Caregiver Support Program Website. The Caregiver Support Program Office advertises the Caregiver Support Program and available mental health support on its website, including information about program eligibility, how to contact program staff, and fact sheets for specific services, such as the Virtual Psychotherapy Program for Caregivers. |
Caregiver Support Program Office officials told us that the Caregiver Support Program webpage had 1.9 million viewers in fiscal year 2025. |
|
Blogs and podcasts. The Caregiver Support Program Office publishes blog stories on its website and podcasts on podcasting platforms about caregivers’ experiences and mental health and wellbeing services. Blog topics included coping with grief and loss, and health and wellbeing coaching for caregivers. Podcast topics included dealing with loneliness and isolation and virtual individual counseling for caregivers. |
The Caregiver Support Program Office published five blogs on its website in 2023, nine blogs in 2024, and nine blogs in 2025, according to program officials. The Caregiver Support Program Office also published four podcasts in 2025 about caregivers’ mental health on podcast platforms, according to agency documentation and officials. |
|
Email lists. The Caregiver Support Program Office sends email updates about the program’s mental health and wellbeing services and caregivers’ experiences through a listserv of about 460,000 individuals who have signed up to receive updates as of May 2025. In addition, program staff we spoke with at two VA medical centers said they send out email newsletters to caregivers enrolled at their facilities to share information about upcoming events and reminders for ongoing local programs. |
The Caregiver Support Program Office sent out 12 email updates in 2023, 17 emails in 2024, and 6 email updates in 2025, according to program officials. Program staff we spoke with at three VA medical centers said they send out monthly newsletters to caregivers. |
|
Partnerships with veterans service organizations and community organizations. Caregiver Support Program Office officials said they brief community partners, including veterans service organizations and caregiver organizations, on mental health services available through the Caregiver Support Program. |
In 2024, Caregiver Support Program Office officials reported they worked with all 50 state veteran commissions, and have briefed 42 state veteran commissions as of May 2025. Caregiver Support Program staff also participate in national events hosted by veterans service organizations. |
|
Resource fairs. Three selected VA medical centers held resource fairs to advertise the Caregiver Support program and services available to caregivers from VHA, local non-profits, and community agencies. |
Caregiver Support Program Office guidance requires program staff at VA medical centers staff to hold a resource fair for caregivers annually.a Three selected VA medical centers we interviewed most recently hosted these fairs in fiscal year 2025, according to medical center documentation. |
|
Wellness contacts. Caregiver Support Program Office guidance directs program staff at VA medical centers to ask caregivers about their mental health and wellbeing needs, during regular, required wellness contacts and share information on available support. Program staff at two VA medical centers we visited provided a packet of information about available resources they provide to caregivers during these visits. |
Caregiver Support Program staff must conduct wellness contacts with caregivers participating in the comprehensive component every 120 days and annually for caregivers enrolled in the general component, according to VHA policy. |
Source: GAO analysis of Department of Veterans Affairs (VA) information. | GAO‑26‑108070
Note: We conducted interviews with officials from the Caregiver Support Program office and Caregiver Support Program staff at four VA medical centers, which we selected based on geography, size of Caregiver Support Program, and rurality.
aResource fairs were put on hold as of January 2025 because of an executive order that has limited their availability to do public facing events, according to Caregiver Support Program Office officials.
In addition to the methods described above, the Caregiver Support Program Office strategic communications plan directs VA medical centers to place informational brochures and other advertising in the medical centers to advertise the Caregiver Support Program and its available mental health support. At two of the VA medical centers we visited in person, we observed physical materials advertising the Caregiver Support Program. Figure 4 shows examples of these materials.
Figure 4: Examples of Informational Brochures and Application Materials for the Caregiver Support Program at Selected Department of Veterans Affairs Medical Centers

Certain methods the Caregiver Support Program Office has used to raise awareness, such as resource fairs and partnerships with community organizations, target caregivers of veterans who are not enrolled or participating in the program. Other methods, like wellness contacts, aim to make sure caregivers who are in the program know about the support available to them. Some caregivers we spoke to at four selected VA medical centers said they became aware of the Caregiver Support Program through each of the methods listed in table 5. Other caregivers cited informal ways of hearing about the program, such as through friends or other veteran families who were aware of the program or were participating in it. Caregivers who learned about the program in these ways often were not seeking out information on the Caregiver Support Program, but were alerted to it by someone who thought they might benefit from it. Further, some of the caregivers we interviewed said they wished they would have become aware of the program sooner in their tenure as caregivers and felt that other caregivers were not aware of the program and the help it can provide.
VHA Has Goals for Its Efforts to Disseminate Information but Does Not Follow Other Performance Management Practices
We found the Caregiver Support Program Office has partially implemented key performance management practices by establishing goals and collecting data related to these goals and the office’s efforts to disseminate information on the program to caregivers. Our prior work defines performance management as a three-step process by which agencies should (1) set goals with quantitative targets and time frames to identify the results they seek to achieve, (2) collect performance information to measure progress towards meeting those goals, and (3) use that information to assess results and inform decisions to ensure further progress towards achieving its goals.[21]
According to the Caregiver Support Program Communications Strategic Plan for fiscal year 2025, the Caregiver Support Program Office aims to increase awareness of the program among caregivers and partners outside of VA, such as veterans service organizations.[22] Within its strategic plan, the Caregiver Support Program Office set goals for its efforts to increase awareness of the program among caregivers. Specifically, the plan states the program aims to increase
· the number of caregivers who are enrolled in the program,
· the number of program inquiries,
· the number of email subscribers who receive updates and program information, and
· caregivers’ use of program services.
The Caregiver Support Program Office also generally collects performance information to measure progress on its goals. Caregiver Support Program Office officials said they collect various data, such as program applications and enrollment to measure the extent to which their outreach is effective. For example, according to these data, the agency met its target to increase program enrollment in the general component in fiscal year 2025, as the number of caregivers enrolled in the general component increased by 15 percent, from about 24,800 caregivers in fiscal year 2024 to about 28,500 in fiscal year 2025. The Caregiver Support Program also collects data on the number of email update subscribers, with about 436,000 subscribers as of May 2025, according to agency data.
According to key performance management practices, the goals an agency sets should have quantifiable targets and time frames within which the targets should be met. We found the Caregiver Support Program Office established one goal with a target to increase program enrollment in the general component by 15 percent each fiscal year. Officials from the Caregiver Support Program Office said they set a target for enrollment in the general component because almost all caregivers of veterans can enroll in it, whereas the comprehensive component has stricter criteria to participate.[23] However, the Caregiver Support Program Office’s other three goals do not have quantitative targets or time frames within which the targets should be met. For example, the program aims to increase the number of subscribers to its email updates but has not defined by how much or when the target should be reached. Officials said they did not develop goals or metrics based on their Communications Strategic Plan but rather based on what they hear from caregivers and program staff. Therefore, Caregiver Support Program officials are not taking steps to fully implement key performance management practices because they have not developed quantitative targets or time frames for its other three goals.
Developing targets and time frames for its other three goals would allow the Caregiver Support Program Office to further define what it is aiming to achieve in increasing caregivers’ awareness of the program. The program can use the information it already collects to measure progress towards its goals and then make any needed adjustments to its outreach activities or revise its goals based on the results. For example, the Caregiver Support Program Office could set a target of a certain percentage increase for its goals to increase email update subscribers each year and use the data it tracks on the number of subscribers to determine if that goal has been met. The program could adjust its outreach strategy to make greater progress towards its target if not met.
Taking these steps would allow the Caregiver Support Program to more effectively assess its outreach efforts and use the results to identify areas where the program can improve its efforts to spread awareness of the program. By doing so, the Caregiver Support Program Office would be better able to determine whether it should adjust its actions to address concerns caregivers expressed. For example, addressing caregivers’ concerns about wanting to learn about the program earlier could help the program provide services to caregivers at an earlier point in their caregiving. These steps could then help the program fulfill its mission to promote the health and wellbeing of caregivers of veterans.
VHA’s Efforts to Assess Mental Health Support Offered by Caregiver Program Follow Some, but Not All, Performance Management Practices
We found the Caregiver Support Program Office has incorporated some key performance management practices in its efforts to assess how effectively the program is supporting caregivers’ mental health. As previously noted, our prior work defines performance management as a three-step process by which agencies (1) set goals with quantitative targets and time frames to identify the results they seek to achieve, (2) collect performance information to measure progress towards meeting those goals, and (3) use that information to assess results and inform decisions to ensure further progress towards achieving its goals.[24]
The Caregiver Support Program Office has taken the first steps to implement these practices. Specifically, in 2024 it established a goal related to one of the services it provides: mental health treatment caregivers receive through the Virtual Psychotherapy Program for Caregivers. Program officials said they set a goal to increase the number of encounters completed through the Virtual Psychotherapy Program for Caregivers by 10 percent from fiscal year 2024 to fiscal year 2025.
|
Caregiver Support Program Information Referrals are requests or recommendations for caregivers to receive a specific service. For example, Caregiver Support Program staff may refer caregivers in the comprehensive component to mental health treatment through the Virtual Psychotherapy Program for Caregivers if they show signs of depression. Staff may also recommend non-clinical program services like support groups and coaching programs, depending on the caregivers’ needs. Encounters include contacts between caregivers and Caregiver Support Program staff or participation in program services, such as individual appointments for mental health treatment or participation in support groups. Encounter data does not include services provided to caregivers by other VHA departments or care provided outside of VHA, according to program officials. Source: GAO analysis of Veterans Health Administration (VHA) information. | GAO‑26‑108070 |
To determine whether the program is meeting this goal, the Caregiver Support Program Office tracks encounter data to see the number and percentage of caregivers that have received mental health treatment through the Virtual Psychotherapy Program for Caregivers. Officials said they use a dashboard to review these data at the national and regional level on a weekly basis to monitor whether use of this service is growing. In fiscal year 2025, the program had met its goal, having increased the number of encounters by over 50 percent from fiscal year 2024 to 2025, according to officials.
In addition, the Caregiver Support Program Office is developing a tool to also track referrals that Caregiver Support Program staff give to caregivers to obtain mental health treatment through the Virtual Psychotherapy Program for Caregivers. In January 2026, officials said they expect to use the tool starting in February 2026 to track referral data across VA medical centers to identify and address any service gaps.
The Caregiver Support Program’s goal for the virtual psychotherapy program is specific to the mental health treatment received through that program, and this goal does not include encounters or referrals outside of the program, such as for mental health treatment at VA medical centers. According to our analysis of VHA data, about one-third of caregivers who received mental health treatment had their appointment through a VA medical center in fiscal year 2025. Officials said they do not have a goal related to mental health treatment outside of the virtual psychotherapy program or collect related data because that mental health treatment is provided by VHA clinicians outside of the Caregiver Support Program.
In addition, the program has not established goals related to other Caregiver Support Program services that support caregivers’ mental health, such as coaching programs or support groups. In January 2026, officials said they had not yet collected enough data on caregivers’ use of these other program services to be able to establish related goals. Officials said they expect to collect baseline data on these other program services through fiscal year 2026 and then will determine whether to set any additional goals.
Starting in 2025, the Caregiver Support Program Office began taking steps to facilitate the collection of information on referrals and encounters for other services the program offers caregivers in both the general and comprehensive components, such as self-care courses or support groups. Specifically, the Caregiver Support Program Office released a template for caregivers’ electronic health records that program staff at VA medical centers are to fill out to document that they referred a caregiver to a certain service. In addition, program staff are to complete this template to document which program services caregivers use. After a caregiver uses a service, program officials said they can track it as an encounter through the electronic health record system, and they then use the documented information from the template to track encounters by the specific type of services caregivers use. Caregiver Support Program Office officials said tracking such referrals and encounters by service type will allow them to see which services caregivers are referred to and using most often. Officials said they identified the need to collect information for specific services as the program has expanded the services it offers.
Establishing goals with quantitative targets and time frames for all of the support services the Caregiver Support Program offers, including coaching and support groups, would allow the program to define what it aims to achieve for all services and then measure its progress towards such goals. For example, setting goals and collecting performance information related to referrals and encounters for mental health treatment provided to caregivers at VA medical centers would provide the program with information to assess overall how well it supports caregivers through mental health treatment. Collecting performance information would also be consistent with VA’s congressionally mandated report to Congress on caregiver support for fiscal year 2024, which stated that identifying and monitoring key performance indicators are essential to maximizing program efficiency and operational effectiveness.[25]
Fully implementing all three performance management steps would also allow the program to determine whether it needs to make any needed adjustments. For example, the Caregiver Support Program Office could set a goal to increase the use of support groups by a certain percentage from the previous fiscal year and use the encounter data it collects to measure progress towards that goal. With this information, staff can make adjustments as needed, such as taking additional steps to follow-up with caregivers who could benefit from attending support groups to support their mental health and wellbeing.
Conclusions
The Caregiver Support Program plays a critical role in supporting caregivers who assist veterans who have suffered serious injuries with essential tasks of everyday living. Given the toll that daily caregiving can take on caregivers’ mental health, ensuring VHA is effectively spreading awareness about the program and the mental health support it offers is essential to ensuring that interested caregivers can participate in the program and receive support. VHA uses various methods to disseminate information about the program and has met one of its goals to increase the number of caregivers participating in the program. However, the other three goals do not have measurable targets and time frames against which the agency could measure its progress in increasing caregivers’ awareness of the program. Developing such targets, as well as following all three performance management practices, would enable VHA to better assess the effectiveness of its outreach efforts to help ensure it is reaching caregivers who need mental health support and make adjustments as appropriate.
Importantly, VHA has also taken steps to assess how well the program supports caregivers’ mental health needs by establishing a goal for the Virtual Psychotherapy Program for Caregivers and collecting information on use of certain program services. By establishing additional goals and collecting data for other services the program offers, VHA would be better positioned to assess how effectively it is meeting the mental health needs of those in the program and make any necessary adjustments. With this information, VA could better understand how program efforts promote the health and wellbeing of caregivers, which helps them to better support veterans.
Recommendations for Executive Action
We are making the following two recommendations to VA:
The Secretary of the Department of Veterans Affairs should ensure the Under Secretary for Health implements key performance management practices to increase the awareness of the Caregiver Support Program by (1) establishing quantitative targets and time frames for all of its program goals, such as increasing the number of program inquiries, and (2) using these data to assess program performance and make adjustments as appropriate. (Recommendation 1)
The Secretary of the Department of Veterans Affairs should ensure the Under Secretary for Health implements key performance management practices to assess the mental health support offered by the Caregiver Support Program by (1) establishing goals with quantitative targets and time frames for all of the mental health support offered through the program, including referrals for mental health care provided at VA medical facilities; (2) collecting performance information to measure progress towards meeting these goals, and (3) using these data to assess program performance and make adjustments as appropriate. (Recommendation 2)
Agency Comments and Our Evaluation
We provided a draft of this report to VA for review and comment. In its written comments, reproduced in appendix II, VA concurred with our recommendations and identified actions VHA plans to take to address them.
Regarding our first recommendation, VA stated that the Caregiver Support Program will establish quantitative targets and time frames for increasing awareness of the program. In addition, VA stated that it will develop tools to measure progress towards such targets and a plan to assess performance periodically. VA estimates it will complete these actions by February 2027.
With respect to our second recommendation, VA stated that it will establish quantitative targets and time frames to monitor mental health services provided through VA medical centers and the Virtual Psychotherapy Program for Caregivers. VA stated that it will develop tools and collect data to measure progress towards such targets and a plan to assess performance periodically. VA estimates it will complete these actions by February 2027.
However, VA did not provide information on whether or how it plans assess the other services it provides to support caregivers’ mental health and wellbeing, such as coaching and support groups. As we reported, VA started to collect data on these services in 2025 but had not established any related goals as of January 2026. By establishing goals with quantitative targets and time frames for other program services beyond mental health treatment, and by using the data it collects to measure progress towards such goals, VA would be better positioned to more comprehensively assess program performance and make any needed adjustments to further support caregivers.
VA also provided technical comments, which we incorporated as appropriate.
We are sending copies of this report to the appropriate congressional committees, the Secretary of Veterans Affairs, and other interested parties. In addition, the report is available at no charge on the GAO website at https://www.gao.gov. If you or your staff have any questions about this report, please contact me at hundrupa@gao.gov. Contact points for our Offices of Congressional Relations and media relations may be found on the last page of this report. GAO staff who made key contributions to this report are listed in appendix III.

Alyssa M. Hundrup
Director, Health Care
The Senator Elizabeth Dole 21st Century Veterans Healthcare and Benefits Improvement Act includes a provision for us to review the Veterans’ Health Administration (VHA) efforts to provide mental health support for caregivers of veterans.[26] In this report, we
1. describe the factors that can affect caregivers’ mental health and wellbeing;
2. describe the mental health support VHA offers caregivers, and actions it has taken to address challenges caregivers may face obtaining support;
3. examine VHA’s efforts to make caregivers aware of the Caregiver Support Program and available mental health support; and
4. examine VHA’s efforts to assess how the Caregiver Support Program is supporting caregivers’ mental health.
To answer our first objective, we conducted a literature search and review to identify factors that can affect caregivers’ mental health and wellbeing. For the literature search, we conducted a structured search of multiple databases using various terms related to our objective, including, “caregiver,” “veteran,” “wellbeing,” “mental health,” and “behavioral health,” among others.[27] We limited search results to English language materials (e.g., peer-reviewed articles and research organization reports), focused on veterans of the United States, and articles published from 2020 through 2025. Our structured search identified 118 articles. An analyst reviewed summary information from each of the 118 articles to determine their relevance to our review. Of the 118 articles, we identified 19 for full-text review.
To review the 19 selected articles, we used a structured format to identify (1) facts presented about caregivers’ mental health, (2) outcomes or factors examined that may affect caregivers’ mental health, (3) the area or population studied (caregivers of U.S. veterans), and (4) the methodology used, including any limitations. One analyst completed the initial review, and a separate analyst independently reviewed the results. Of the 19 articles reviewed, we determined 16 were methodologically sound and relevant to our objective. See the bibliography of articles from our structured search at the end of this report.
In addition, we interviewed Caregiver Support Program staff from a nongeneralizable selection of four Department of Veterans Affairs (VA) medical centers and conducted eight discussion groups with 50 selected caregivers who are participating in the program at these VA medical centers to understand caregivers’ mental health and factors that can affect their health and wellbeing. We selected these VA medical centers for variation in geography, rurality, and the number of caregivers participating in the Caregiver Support Program.[28] We worked with VA medical center staff to conduct outreach to caregivers to participate in these discussion groups. Specifically, VA medical center staff sent a flyer to caregivers participating in each program component advertising the discussion group and opportunity to share their experiences with GAO.[29] Caregivers participated in these discussions in person at the selected VA medical centers and remotely (e.g., via telephone or VA Video Connect). We held anonymous discussion groups without VA medical center staff present.
We also interviewed officials from two veterans service organizations and two foundations that serve veterans and their caregivers about caregivers’ mental health conditions and factors that contribute to them.[30] We selected these organizations and foundations based on their focus on caregivers of veterans, knowledge of the Caregiver Support Program, and national reach. Information we obtained from these discussion groups and interviews is not generalizable across caregivers or VA medical centers; however, the information we obtained from them illustrates a variety of experiences from caregivers and staff.
To answer our second objective, we reviewed VHA documentation that describes the mental health support it offers caregivers, such the Caregiver Support Program website and fact sheets. We also reviewed VHA guidance for VA medical center staff on how they should address challenges caregivers face, such as Caregiver Support Program field guides.
In addition, we obtained data from VHA for fiscal years 2021 through 2025 on participating caregivers’ usage of the program. We reviewed data starting in fiscal year 2021, because eligibility for the Caregiver Support Program expanded significantly in that year, through 2025, the most recent complete fiscal year of data.[31] We obtained data on the number of caregivers participating in the comprehensive component that received mental health treatment.[32] We also obtained data and the number of caregivers that had a mental health diagnosis documented in their electronic health record.[33] The number of caregivers that received mental health treatment includes caregivers active in the comprehensive component each fiscal year and had at least one mental health encounter at a Department of Veterans Affairs (VA) facility or through the Virtual Psychotherapy Program for Caregivers.[34]
The number of caregivers with mental health diagnoses includes the three most common groups VHA identified among caregivers: depression-related disorders, anxiety-related disorders, and post-traumatic stress disorder. These groups include specific, related diagnoses. For example, depression-related disorders include recurring and single episodes of major depressive disorder, and anxiety-related disorders include generalized anxiety disorder and other disorders, such as phobias. We calculated the percentage of caregivers with a mental health diagnosis by dividing the number of caregivers with each diagnosis group by the number of caregivers with at least one mental health encounter for each fiscal year. According to Caregiver Support Program Office officials, only caregivers who had a mental health encounter (i.e., received mental health treatment) would have a diagnosis in their electronic health record.
We also used data from VHA to describe characteristics of caregivers enrolled or participating in the Caregiver Support Program for fiscal years 2021 through 2025. Specifically, we obtained data on the number of caregivers enrolled or participating in the program by sex, age groups, and relationship to the veteran for the general and comprehensive components for each fiscal year.[35] We divided the number of caregivers in each demographic group by the number of caregivers enrolled or participating in the program to calculate percentages.
To assess the reliability of the VHA data we obtained, we reviewed agency documentation, such as guidance for VA medical center staff who collect this information from caregivers, interviewed relevant agency officials and reviewed written responses from agency officials, to better understand the data. We also tested the data for errors. On the basis of these steps, we determined the data were sufficiently reliable for the purposes of our reporting objectives.
In addition, we interviewed VHA officials from the national Caregiver Support Program Office who are responsible for overseeing the program and providing guidance to VA medical centers implementing the program. We interviewed these officials to understand what mental health support VHA offers to caregivers and any actions VHA has taken to address challenges caregivers face. Further, we interviewed Caregiver Support Program staff and participating caregivers at the four selected VA medical centers about the mental health support offered at their medical center and any challenges caregivers faced obtaining support. Information we obtained from these interviews is not generalizable across caregivers or VA medical centers; however, the information we obtained from them illustrates a variety of experiences from caregivers and staff. We also observed program operations at three of the four selected medical centers to understand the mental health support offered, such as observing where staff hold support groups and a call center from which staff contact caregivers.[36]
To answer our third objective, we reviewed VHA documentation that describes its processes for spreading awareness of the program and available mental health support, such as field guides for VA medical center staff who administer the program locally and the Caregiver Support Program’s Communications Strategic Plan for fiscal year 2025. In addition, we interviewed Caregiver Support Program Office officials and staff at the four selected VA medical centers to understand their efforts to spread awareness of the program, such as sending out email newsletters. We also interviewed caregivers participating in the program at these VA medical centers to obtain their perspectives on VHA’s efforts to spread awareness, including how they became aware of the program. Information we obtained from these interviews is not generalizable across caregivers or VA medical centers; however, the information we obtained from them illustrates a variety of experiences from caregivers and staff. Further, we observed program operations at three of the four selected medical centers to identify advertising for the Caregiver Support Program, such as signage and program pamphlets.[37] We used this information to evaluate the Caregiver Support Program Office’s efforts to assess how it disseminates information on the program against performance management criteria we identified in prior work to determine the extent to which these efforts are consistent with key performance management practices.[38]
To answer our fourth objective, we reviewed VHA documentation that describes how it collects information on Caregiver Support Program services, such as a template for VA medical center staff to document caregivers’ referrals and encounters in their electronic health record. In addition, we interviewed Caregiver Support Program Office officials and staff, and reviewed officials’ written responses, about their efforts to assess how the program is supporting caregivers’ mental health, such as identifying what data the program tracks on caregivers’ use of program services. We used this information to evaluate the Caregiver Support Program Office’s efforts against VA’s Congressionally Mandated Report on caregiver support for fiscal year 2024 and performance management criteria we identified in prior work to determine the extent to which these efforts are consistent with key performance management practices.[39]


Alyssa M. Hundrup, hundrupa@gao.gov
In addition to the contact named above, Rebecca Rust Williamson (Assistant Director), Erika Huber (Analyst-in-Charge), Mikayla Ferg, and Megan Knox made key contributions to this report. Also contributing were Leia Dickerson, David Jones, Diona Martyn, Monica Perez-Nelson and Cathleen Whitmore.
Brickell, Tracey A., Megan M. Wright, Jamie K. Sullivan, et al. “Health Outcomes in Caregivers of Service Members and Veterans With Traumatic Brain Injury Enrolled in the U.S. Veterans Affairs Caregiver Support Program.” Psychological Services, vol. 21, no. 3 (2024): 635-648.
Carlozzi, Noelle E., Rael T. Lange, Nicholas R. Boileau, et al. “TBI-CareQOL Family Disruption: Family Disruption in Caregivers of Persons With TBI.” Rehabilitation Psychology, vol. 65, no. 4 (2020): 390-400.
Delgado, Roxana E., Kimberly Peacock, Chen-Pin Wang, and Mary Jo Pugh. “Phenotypes of Caregiver Distress in Military and Veteran Caregivers: Suicidal Ideation Associations.” PloS One, vol. 16, no. 6 (2021): 1-15.
Gandhi, Priya, Kayla M. Williams, and Rajeev Ramchand. Perspectives of America’s Military and Veteran Caregivers: A Qualitative Exploration. Santa Monica, Calif.: RAND Corporation, 2024.
Harrod, Molly, Katrina Hauschildt, Lee A. Kamphuis, et al. “Disrupted Lives: Caregivers’ Experiences of In-Hospital Cardiac Arrest Survivors’ Recovery 5 Years Later.” Journal of the American Heart Association, no. 18, vol. 12 (2023): 1-10.
Henion, Amy, Amanda Cheney, Mary Jo Pugh, et al. “Women Veterans as caregivers: Characteristics and comparisons with women non-veterans using BRFSS.” Journal of Women & Aging, vol. 36, no. 6 (2024): 534-545.
Jabbarinejad, Roxana, Shira Cohen-Zimerman, Amy K. Wagner, and Jordan Grafman. “Determinants of Caregiver Burden in Male Patients with Epilepsy Following Penetrating Traumatic Brain Injury.” Epilepsy & Behavior, vol. 116 (2021): 107768.
Jones, Lindsey A., Elisa J. Gordon, Timothy P. Hogan, et al. “Challenges, Facilitators, and Recommendations for Implementation of Home Dialysis in the Veterans Health Administration: Patient, Caregiver, and Clinician Perceptions.” Kidney360, vol. 2 (2021): 1928-1944.
Miller, Katherine E.M., Courtney H. Van Houtven, Erin E. Kent, et al. “Short-term Effects of Comprehensive Caregiver Supports on Caregiver Outcomes.” Health Services Research, vol. 58 (2023): 140-153.
Nicholas, Linda O., Jennifer Martindale-Adams, Ronald T. Seel, Jeffrey K. Zuber, and Paul B. Perrin. “Demographics, Clinical Characteristics, and Well-Being of Veterans with TBI and Dementia and Their Caregivers.” Geriatrics, vol. 9, no. 130 (2024): 1-14.
Ramchand, Rajeev, Sarah Dalton, Tamara Dubowitz, et al. America’s Military and Veteran Caregivers: Hidden Heroes Emerging from the Shadows. Santa Monica, Calif.: RAND Corporation, 2024.
Ramchand, Rajeev, Sarah Dalton, Tara Dubowitz, et al. America’s Military and Veteran Caregivers: What Has Changed from 2014 to 2024, and What Still Needs to Be Done? Santa Monica, Calif.: RAND Corporation, 2024.
Ramchand, Rajeev, Sarah Dalton, Tamara Dubowitz, et al. Nine Ways to Improve the Health and Well-Being of America’s Military and Veteran Caregivers. Santa Monica, Calif.: RAND Corporation, 2024.
RAND Corporation. “The Value of Caregivers to Veterans’ Health, Wellness, and Recovery.” Research & Commentary. Last modified November 6, 2024. https://www.rand.org/pubs/articles/2024/the-value-of-caregivers-to-veterans-health-wellness.
Sander, Angelle M., Nicholas R. Boileau, Robin A. Hanks, David S. Tulsky, and Noelle E. Carlozzi. “Emotional Suppression and Hypervigilance in Military Caregivers: Relationship to Negative and Positive Affect.” Journal of Head Trauma Rehabilitation, vol. 35, no. 1 (2020): E10-E20.
Swabe, Gretchen, Thomas E. Trail, and Rajeev Ramchand. America’s Military and Veteran Caregivers: Hidden Heroes Emerging from the Shadows: Annex of Estimates with Associated 95 Percent Confidence Intervals. Santa Monica, Calif.: RAND Corporation, 2024.
The Government Accountability Office, the audit, evaluation, and investigative arm of Congress, exists to support Congress in meeting its constitutional responsibilities and to help improve the performance and accountability of the federal government for the American people. GAO examines the use of public funds; evaluates federal programs and policies; and provides analyses, recommendations, and other assistance to help Congress make informed oversight, policy, and funding decisions. GAO’s commitment to good government is reflected in its core values of accountability, integrity, and reliability.
Obtaining Copies of GAO Reports and Testimony
The fastest and easiest way to obtain copies of GAO documents at no cost is through our website. Each weekday afternoon, GAO posts on its website newly released reports, testimony, and correspondence. You can also subscribe to GAO’s email updates to receive notification of newly posted products.
Order by Phone
The price of each GAO publication reflects GAO’s actual cost of production and distribution and depends on the number of pages in the publication and whether the publication is printed in color or black and white. Pricing and ordering information is posted on GAO’s website, https://www.gao.gov/ordering.htm.
Place orders by calling (202) 512-6000, toll free (866) 801-7077,
or
TDD (202) 512-2537.
Orders may be paid for using American Express, Discover Card, MasterCard, Visa, check, or money order. Call for additional information.
Connect with GAO
Connect with GAO on X,
LinkedIn, Instagram, and YouTube.
Subscribe to our Email Updates. Listen to our Podcasts.
Visit GAO on the web at https://www.gao.gov.
To Report Fraud, Waste, and Abuse in Federal Programs
Contact FraudNet:
Website: https://www.gao.gov/about/what-gao-does/fraudnet
Automated answering system: (800) 424-5454
Media Relations
Sarah Kaczmarek, Managing Director, Media@gao.gov
Congressional Relations
David A. Powner, Acting Managing Director, CongRel@gao.gov
General Inquiries
[1]Mental health includes emotional, psychological, and social wellbeing, according to the Substance Abuse and Mental Health Services Administration. For purposes of this report, we define mental health to include psychological conditions, such as anxiety-related disorders, and factors related to overall wellbeing, such as stress.
For example, see Megan Shepherd‐Banigan et al., "Family Caregivers of Veterans Experience High Levels of Burden, Distress, and Financial Strain," Journal of the American Geriatrics Society, vol. 68, no. 11 (2020): 2675-2683; Linda O. Nicholas et al., “Demographics, Clinical Characteristics, and Well-Being of Veterans with TBI and Dementia and Their Caregivers,” Geriatrics, vol. 130, no. 9 (2024): 1-14; and Rajeev Ramchand et al., America’s Military and Veteran Caregivers: Hidden Heroes Emerging from the Shadows, (Santa Monica, Calif.: RAND Corporation, 2024).
[2]Ramchand, America's Military and Veteran Caregivers.
[3]Pub. L. No. 118-210, § 131, 138 Stat. 2706, 2741 (2025).
[4]We conducted a structured search of peer-reviewed articles and research organization reports using various terms related to our objective, such as “caregiver,” “veteran,” and “mental health.” We reviewed the facts presented, population studied, and methodology used, including any limitations, and identified 16 articles that were relevant and methodologically sound.
[5]We interviewed Caregiver Support Program staff at VA medical centers located in Long Beach, California; Hines, Illinois; Manchester, New Hampshire; and Lexington, Kentucky. We also conducted in-person site visits to three of the selected VA medical centers (Long Beach, California; Hines, Illinois; and Manchester, New Hampshire) and observed Caregiver Support Program operations, such as staff call centers.
[6]We interviewed officials from Disabled American Veterans, Paralyzed Veterans of America, Elizabeth Dole Foundation, and Quality of Life Foundation.
[7]GAO, Evidence-Based Policymaking: Practices to Help Manage and Assess the Results of Federal Efforts, GAO‑23‑105460 (Washington, D.C.: July 12, 2023).
[9]Pub. L. No. 111-163, § 101, 124 Stat. 1130, 1132 (codified at 38 U.S.C. § 1720G).
[10]In this report, we use the term Caregiver Support Program to refer to both components of the program, unless specifically noted otherwise.
[11]According to VHA data for fiscal year 2025, the Caregiver Support Program received about 66,000 applications from caregivers to participate in the comprehensive component and approved about 30 percent of those applications. The Caregiver Support Program Office denied the remaining 70 percent of applications due to clinical reasons, such as the veteran not needing personal care services for at least 6 continuous months.
[12]See 38 C.F.R. § 71.40 (2024).
[13]In June 2022, VA paused regular, annual reassessments. In September 2025, VA extended the pause through September 2028, while it reviews the effects of legislative and regulatory changes to caregivers’ eligibility for the comprehensive component.
[14]Pub. L. No. 115-182, § 161, 132 Stat. 1393, 1438. The VA MISSION Act of 2018 expanded eligibility for the comprehensive component to veterans who served on or before September 11, 2001; prior to that time, the comprehensive component was limited to veterans who served on or after September 11, 2001.
[15]Caregiver Support Program Office officials noted that program growth has exceeded their estimates at times. In 2014, we reported that VHA initially underestimated the number of caregivers the Caregiver Support Program would serve in the comprehensive component, which resulted in insufficient staffing to operate the program at VA medical centers. We recommended that VA expedite implementation of an information technology system to track workload data, identify solutions to alleviate workload issues, and use data from the new system to assess the program and make changes as needed. VA implemented these recommendations in 2015, 2019, and 2020. See GAO, VA Health Care: Actions Needed to Address Higher-Than-Expected Demand for the Family Caregiver Program, GAO‑14‑675. (Washington, D.C.: Sept. 18, 2014).
[16]VA’s budget submission includes requests for the upcoming fiscal year and an advanced appropriation for the following fiscal year.
[17]For example, in fiscal year 2025, VA obligated $2.6 billion for the Caregiver Support Program, according to VA officials. About $1.8 billion (72 percent) of those obligations were for monthly stipends, travel benefits, and Civilian Health and Medical Program of the Department of Veterans Affairs health benefits coverage for caregivers in the comprehensive component.
[18]The Caregiver Support Program does not offer mental health treatment to caregivers participating in the general component of the caregiver program, unless it is necessary to support the veteran’s treatment, such as couples’ counseling, or if they are veterans eligible for and receiving health care through VHA.
[19]Veterans may qualify for community care—care provided by non-VHA providers but paid for by VHA—if the needed service is not offered by VHA or if VHA cannot provide the service within a designated time frame or distance from the veteran’s home. According to VHA data, approximately 350 caregivers who were also veterans had a mental health encounter in the community through this program in fiscal year 2025.
[20]The Caregiver Support Program Office estimated the demand for individual mental health treatment among caregivers in the general component by applying mental health treatment utilization rates in fiscal year 2025 among caregivers in the comprehensive component to the number of caregivers enrolled in the general program in fiscal year 2025 over the next 10 fiscal years.
[22]The Caregiver Support Program Communications Strategic Plan includes other strategic objectives that are not directly related to spreading awareness of the program to caregivers of veterans. For example, one objective is to nourish a positive morale among staff.
[23]A caregiver of a veteran is eligible for the general component as long as the veteran is enrolled in VHA health care and the caregiver is at least 18 years old.
[25]Department of Veterans Affairs, Congressionally Mandated Report: Assistance and Support Services for Caregivers Fiscal Year 2024 (Washington, D.C.: June 2025).
[26]Pub. L. No. 118-210, § 131, 138 Stat. 2706, 2741 (2025).
[27]The databases we searched included BIOSIS Previews®, Embase®, MEDLINE®, NTIS, PAIS International, APA PsycINFO®, Scopus, ProQuest, CINAHL with Full Text, EconLit with Full Text, Index to Legal Periodicals Retrospective: 1908-1981, Business Abstracts with Full Text, Business Continuity & Disaster Recovery Reference Center, Risk Management Reference Center, WorldCat, and Harvard Think Tank Search.
[28]We selected VA medical centers located in Long Beach, California; Hines, Illinois; Manchester, New Hampshire; and Lexington, Kentucky. We also conducted in-person site visits to three of the selected VA medical centers (Long Beach, California; Hines, Illinois; and Manchester, New Hampshire) and observed Caregiver Support Program operations, such as staff call centers.
[29]The Caregiver Support Program consists of two separate components: the Program of General Caregiver Support Services (general component) and the Program of Comprehensive Assistance for Family Caregivers (comprehensive component). Caregivers of any eligible veteran enrolled in VA health care may enroll in the general component. Caregivers must apply for the comprehensive component and meet certain criteria (e.g., the veteran must meet a certain level of need) to participate.
[30]We interviewed officials from Disabled American Veterans, Paralyzed Veterans of America, Elizabeth Dole Foundation, and Quality of Life Foundation.
[31]We reviewed VHA data for fiscal year 2020 but did not include these data in our analysis. According to VHA officials, data for years prior to fiscal year 2021 are not comparable, because eligibility for the program expanded significantly in fiscal year 2021 to include a more diverse group of caregivers, thus the population of caregivers the program served prior to fiscal year 2021 is not comparable.
[32]VHA data on mental health treatment and diagnoses do not include caregivers in the general component because these caregivers are not eligible to receive mental health treatment.
[33]Caregivers have an electronic health record in VHA’s system, separate from the veteran.
[34]Caregivers who are also veterans may be eligible to receive mental health treatment in the community. We reviewed data on the number of caregivers with an encounter for mental health treatment in the community; however, we did not include these data in our analysis, because these caregivers are eligible for such treatment due to their veteran status and not through the Caregiver Support Program.
[35]We combined the number of caregivers who are a spouse or significant other into one group. We also combined grandchildren, other relatives, friends, or neighbors, as well as other or unknown relationships, into one group due to the small number of caregivers in each group. In fiscal year 2025, about 2 percent of caregivers in the general component and no caregivers in the comprehensive component had an unknown relationship to the veteran.
[36]We conducted in-person site visits to three VA medical centers (Long Beach, California; Hines, Illinois; and Manchester, New Hampshire).
[37]We conducted in-person site visits to three of the selected VA medical centers (Long Beach, California; Hines, Illinois; and Manchester, New Hampshire) and observed Caregiver Support Program operations, such as staff call centers.
[38]GAO, Evidence-Based Policymaking: Practices to Help Manage and Assess the Results of Federal Efforts, GAO‑23‑105460 (Washington, D.C.: July 12, 2023).
[39]See Department of Veterans Affairs, Congressionally Mandated Report: Assistance and Support Services for Caregivers Fiscal Year 2024 (June 2025) and GAO‑23‑105460.
